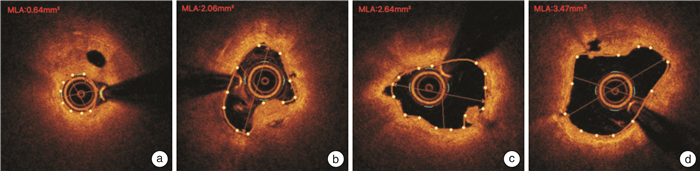
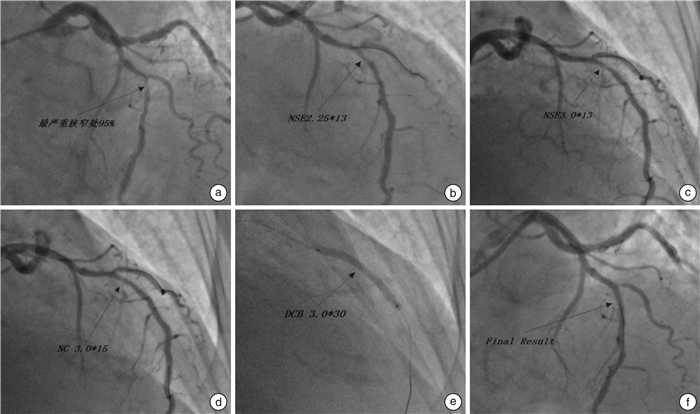
Difference between CAG and OCT in evaluating the changes of coronary lumen during PCI with DCB
-
摘要: 目的 探索冠状动脉(冠脉)原位病变预处理成功的光学相干断层成像技术(OCT)标准及OCT在冠脉原位病变精准介入中的临床价值。方法 选取2020年9月—2021年7月上海交通大学医学院附属第九人民医院冠脉造影(CAG)后需要血运重建,适合行经皮冠脉介入且倾向非植入,并同意行OCT检查的冠心病患者,共30例(31处病变)。在应用控制性球囊成形术作为预处理手段前后,及行药物涂层球囊或药物洗脱支架植入后分别行OCT检查,将OCT与CAG的检查数据及指导的治疗决策进行对比,观察术中预处理成功率及OCT指导的治疗决策转变。结果 按照CAG标准,有28处(90.3%)病变预处理成功;3处(9.7%)病变预处理失败,其中1处病变出现弹性回缩,2处病变出现C型夹层。按照OCT标准,有15处(48.4%)病变预处理成功;16处(52.6%)病变因出现预处理后发生的夹层预处理失败。两种预处理成功标准的治疗策略有统计学差异(P< 0.001)。OCT指导的残余狭窄最小管腔参考直径比CAG指导的残余狭窄最小管腔参考直径更大,且有统计学差异[(2.93±0.07) mm∶(2.77±0.26) mm,P< 0.001]。结论 OCT在指导冠脉原位病变介入治疗时更加精准明确客观,具有较高的临床应用价值。
-
关键词:
- 光学相干断层成像技术 /
- 控制性球囊成形术 /
- 药物涂层球囊 /
- 冠状动脉造影
Abstract: Objective To explore the criteria of optical coherence tomography for the successful pretreatment of coronary artery in situ lesion and observe the clinical value of optical coherence tomography in the precise intervention of coronary in situ lesions.Methods From September, 2020 to July, 2021, 30 patients with coronary heart disease(except for acute ST segment elevation myocardial infarction within 1 month) who needed revascularization after coronary angiography and suitable for coronary intervention(PCI) and predisposed to non-implantation therapy and agreed to accept OCT examination were selected in the Department of Cardiology of Ninth People's Hospital of School of Medicine of Shanghai Jiaotong University. OCT was performed before and after pretreatment, and after drug-coated balloon or drug-eluting stent implantation. The data and treatment decision guided by OCT and coronary angiography were compared. And then we observed the success rate of pretreatment and the change of treatment decision guided by OCT.Results Among the 30 patients and 31 lesions, according to the criteria of coronary arteriography, 28(90.3%) lesions were pretreated successfully, and 3 Lesions failed to be pretreated, in which one(3.2%) lesion showed elastic retraction, and 2 lesions(6.5%) showed type C dissection. According to the criteria of OCT, 15(48.4%) lesions were pretreated successfully, and 16(52.6%) lesions failed to be pretreated due to dissection appeared after pretreatment. There was a significant difference in treatment decision-making between the two pretreatment success criteria(P< 0.001). The Minimum reference diameter of residual stenosis guided by OCT was larger than that guided by coronary angiography(2.93 ± 0.07 mm vs. 2.77 ± 0.26 mm,P=0.002).Conclusion OCT is more accurate, definite, objective and has higher clinical value than coronary angiography in guiding PCI. -

-
表 1 OCT最小管腔面积标准
Table 1. Minimum lumen area standard for OCT
冠脉内径/mm DCB/mm2 DES/mm2 2.5 ≥2.4 < 2.4 3.0 ≥3.5 < 3.5 3.5 ≥4.6 < 4.6 4.0 ≥5.7 < 5.7 表 2 基线特征
Table 2. Baseline characteristics
X±S 项目 数值 患者/例 30 年龄/岁 65.9±7.1 男性/例(%) 22(73.3) 合并疾病/例(%) 高血压 21(70.0) 糖尿病 10(33.3) 高血脂 16(53.3) 甲状腺功能亢进 1(3.3) TIA 1(3.3) 肾功能不全 0(0) 吸烟史 11(36.7) 临床表现/例(%) NSTEMI 5(16.7) SAP 3(10.0) UA 22(73.3) 靶血管/处(%) LAD 20(64.5) RCA 4(12.9) LCX 6(19.4) D1 1(3.2) 靶血管病变位置/处(%) 近段 12(38.7) 中段 12(38.7) 远段 6(19.4) 开口 1(3.2) 注:TIA:短暂性脑缺血;NSTEMI:非ST段抬高型心肌梗死;UA:不稳定型心绞痛;SAP:稳定型心绞痛;LAD:左前降支;LCX:左回旋支;RCA:右冠;D1:第1对角支。 表 3 病变及术中数据
Table 3. Lesion and procedure characteristics
例(%), X±S 项目 OCT提示预处理成功(15例) OCT提示预处理失败(13例) CAG+OCT均提示预处理失败(3例) P值 靶血管 LAD 10(66.7) 7(53.8) 3(100.0) RCA 2(13.3) 4(30.8) 0(0) LCX 2(13.3) 2(15.4) 0(0) D1 1(6.7) 0(0) 0(0) 靶位置 近段 5(33.3) 5(38.5) 2(66.7) 中段 4(26.7) 7(53.8) 1(33.3) 远段 5(33.3) 1(7.7) 0(0) 开口 1(6.7) 0(0) 0(0) 病变分型 A 6(40.0) 8(61.5) 0(0) B 6(40.0) 3(23.1) 2(66.7) C 3(20.0) 2(15.4) 1(33.3) 病变长度/mm 8.53±3.6 9.54±5.0 13.33±7.6 0.270 QCA数据 预处理前DS/% 89.80±7.98 86.38±7.73 93.00±7.21 0.325 预处理后DS/% 21.67±7.94 20.77±8.62 53.33±25.17 < 0.001 参考直径/mm 2.68±0.29 2.81±0.22 3.00±0.00 0.117 OCT数据 预处理前MLA/mm2 1.06±0.54 1.31±0.52 0.69±0.09 0.148 预处理后MLA/mm2 3.49±1.14 3.38±0.67 2.68±0.72 0.401 参考直径/mm 2.82±0.48 3.08±0.30 3.00±0.00 0.221 夹层类型 无 5(33.3) 0(0) 0(0) 内膜 10(66.7) 0(0) 0(0) 中膜 0(0) 13(100.0) 3(100.0) 斑块性质 脂质 12(80.0) 10(76.9) 3(100.0) 纤维 10(66.7) 12(92.3) 2(66.7) 钙化 7(46.7) 9(69.2) 2(66.7) 预处理 预处理球囊平均长度/mm 11.27 11.46 11.67 0.948 预处理球囊平均尺寸/mm 2.78±0.40 2.96±0.30 2.92±0.14 0.401 预处理球囊平均最高充盈压/atm 9.40±2.2 9.08±1.3 9.33±2.3 0.900 预处理球囊 切割球囊 10(66.7) 6(46.2) 3(100.0) 棘突球囊 5(33.3) 6(46.2) 0(0) 非顺应性球囊 0(0) 1(7.7) 0(0) 治疗方式 DCB 15 0 0 DES 0 13 3 DCB或DES平均长度/mm 23.13±4.16 24.46±3.80 24.67±11.55 0.744 DCB或DES平均尺寸/mm 2.77±0.39 2.98±0.33 3.17±0.29 0.134 DCB或DES平均释放压力/atm 7.87±0.8 11.08±2.7 10.00±0.0 < 0.001 DCB平均释放时间/s 59±3.87 - - DES后贴壁情况 CAG表现良好 - 13(100.0) 3(100.0) OCT表现良好 - 4(30.8) 1(33.3) 注:DS:管腔狭窄;MLA:最小管腔横截面积;-:数据缺如。 -
[1] Jeger RV, Farah A, Ohlow MA, et al. Drug-coated balloons for small coronary artery disease(BASKET-SMALL 2): an open-label randomised non-inferiority trial[J]. Lancet, 2018, 392(10150): 849-856. doi: 10.1016/S0140-6736(18)31719-7
[2] 韩旭飞, 刘恒道, 邢军辉, 等. 单纯使用药物涂层球囊治疗冠状动脉慢性完全闭塞性病变的临床疗效分析[J]. 临床心血管病杂志, 2021, 37(7): 604-609. https://www.cnki.com.cn/Article/CJFDTOTAL-LCXB202107004.htm
[3] Scheller B, Vukadinovic D, Jeger R, et al. Survival after coronary revascularization with paclitaxel-coated balloons[J]. J Am Coll Cardiol, 2020, 75(9): 1017-1028. doi: 10.1016/j.jacc.2019.11.065
[4] 侯俐, 卢丽丽, 曾华甦, 等. 切割球囊在药物涂层球囊治疗冠脉原位病变时的临床价值[J]. 老年医学与保健, 2021, 27(3): 590-593. doi: 10.3969/j.issn.1008-8296.2021.03.034
[5] Räber L, Mintz GS, Koskinas KC, et al. 冠状动脉内影像学临床应用专家共识(第一部分): 对冠状动脉介入治疗的指导与优化[J]. 中华心血管病杂志, 2019, 47(1): 5-25.
[6] Chung JH, Lee KE, Her AY, et al. Comparison of fractional flow reserve and angiographic characteristics after balloon angioplasty in de novo coronary lesions[J]. Int J Cardiovasc Imaging, 2019, 35(11): 1945-1954. doi: 10.1007/s10554-019-01649-y
[7] Kuku KO, Ekanem E, Azizi V, et al. Optical coherence tomography-guided percutaneous coronary intervention compared with other imaging guidance: a meta-analysis[J]. Int J Cardiovasc Imaging, 2018, 34(4): 503-513. doi: 10.1007/s10554-017-1272-2
[8] Johnson TW, Räber L, di Mario C, et al. Clinical use of intracoronary imaging. Part 2: acute coronary syndromes, ambiguous coronary angiography findings, and guiding interventional decision-making[J]. Eur Heart J, 2019, 40(31): 2566-2584. doi: 10.1093/eurheartj/ehz332
[9] Räber L, Mintz GS, Koskinas KC, et al. Clinical use of intracoronary imaging. Part 1: guidance and optimization of coronary interventions[J]. Eur Heart J, 2018, 39(35): 3281-3300. doi: 10.1093/eurheartj/ehy285
[10] Kume T, Uemura S. Current clinical applications of coronary optical coherence tomography[J]. Cardiovasc Interv Ther, 2018, 33(1): 1-10. doi: 10.1007/s12928-017-0483-8
[11] Leistner DM, Riedel M, Steinbeck L, et al. Real-time optical coherence tomography coregistration with angiography in percutaneous coronary intervention-impact on physician decision-making: The OPTICO-integration study[J]. Catheter Cardiovasc Interv, 2018, 92(1): 30-37. doi: 10.1002/ccd.27313
[12] Prati F, Romagnoli E, La Manna A, et al. Long-term consequences of optical coherence tomography findings during percutaneous coronary intervention: the Centro Per La Lotta Contro L'infarto-Optimization of Percutaneous Coronary Intervention(CLI-OPCI)LATE study[J]. EuroIntervention, 2018, 14(4): e443-e451. doi: 10.4244/EIJ-D-17-01111
[13] Häner JD, Duband B, Ueki Y, et al. Impact of intracoronary optical coherence tomography in routine clinical practice: A contemporary cohort study[J]. Cardiovasc Revasc Med, 2021, Jul 27, S1553-8389(21)00559-5.
[14] Kubo T, Ino Y, Shiono Y, et al. Usefulness of optical coherence tomography with angiographic coregistration in the guidance of coronary stent implantation[J]. Heart Vessels, 2021, Jul 21, doi: 10.1007/s00380-021-01911-1.
[15] Schneider VS, Böhm F, Blum K, et al. Impact of real-time angiographic co-registered optical coherence tomography on percutaneous coronary intervention: the OPTICO-integration Ⅱ trial[J]. Clin Res Cardiol, 2021, 110(2): 249-257. doi: 10.1007/s00392-020-01739-1
[16] Ziad AA, Keyvan KG, Gary SM, et al. Intracoronary optical coherence tomography: state of the art and future directions[J]. Euro Intervention, 2021, 17(2): e105-e123.
-




 下载:
下载: