Changes of vWF、NLR、MPVLR in HFrEF patients with type 2 diabetes mellitus and its clinical significance
-
摘要: 目的 探讨射血分数降低型心力衰竭(HFrEF)合并2型糖尿病(T2DM)患者血管性血友病因子(vWF)、中性粒细胞/淋巴细胞比值(NLR)、平均血小板体积/淋巴细胞比值(MPVLR)等微血管炎症指标的变化水平及三者在HFrEF患者中的预测价值。方法 连续入选石河子大学医学院第一附属医院2021年3月—2022年3月在心内科住院治疗的HFrEF患者100例,根据有无合并T2DM分为HFrEF组(50例)和HFrEF-T2DM组(50例),另外选取同期除外心力衰竭和T2DM的心血管疾病患者50例作为对照组。收集所有患者的一般资料、血常规、生化、超声心动图等指标,计算NLR、MPVLR,酶联免疫吸附法测定各组患者血清vWF水平;同时分析3个指标与左心室射血分数(LVEF)、N末端B型利钠肽(NT-proBNP)的相关性;ROC曲线分析3个指标在HFrEF患者中的预测价值。结果 与对照组比较,HFrEF组和HFrEF-T2DM组患者的vWF、NLR、MPVLR水平升高(P< 0.001);与HFrEF组比较,HFrEF-T2DM组患者的vWF、NLR、MPVLR水平升高更为显著(P< 0.001)。相关性分析显示,血清vWF、NLR、MPVLR与LVEF呈负相关(r=-0.510、-0.403、-0.324,P< 0.001),与NT-proBNP呈正相关(r=0.616、0.453、0.343,P< 0.001)。ROC曲线分析显示,MPVLR预测HFrEF患者炎症损伤的灵敏度最高,vWF特异度最高。结论 vWF、NLR、MPVLR在HFrEF合并T2DM中存在较高的激活水平,其可能成为预测疾病严重程度的重要参考指标。
-
关键词:
- 射血分数降低型心力衰竭 /
- 2型糖尿病 /
- 血管性血友病因子 /
- 中性粒细胞/淋巴细胞比值 /
- 平均血小板体积/淋巴细胞比值
Abstract: Objective To investigate the changes in vascular inflammation indexes such as von willebrand factor (vWF), neutrophil-to-lymphocyte ratio (NLR), and mean platelet volume-to-ymphocyte ratio (MPVLR) in patients with HFrEF combined with type 2 diabetes mellitus (T2DM) and their predictive values.Methods A total of 100 HFrEF patients hospitalized in the department of Cardiology of The First Affiliated Hospital, School of Medicine, Shihezi University from March 2021 to March 2022 were enrolled and divided into the HFrEF group (n=50) and HFrEF-T2DM group (n=50) according to whether T2DM was present. In addition, 50 patients with cardiovascular disease excluding heart failure and T2DM were selected as the control group during the same period. The general data, blood routine, biochemical, echocardiography, and other indicators of all patients were collected. NLR and MPVLR were calculated. The serum vWF level of each group was determined by enzyme-linked immunosorbent assay. The correlation between the three factors and left ventricular ejection fraction (LVEF), and N-terminal brain natriuretic peptide (NT-proBNP) were analyzed. ROC curve was used to analyze the predictive value of the three factors in all HFrEF patients.Results Compared with the control group, vWF, NLR, MPVLR levels in HFrEF group and HFrEF-T2DM group were significantly increased (P< 0.001); vWF, NLR, MPVLR levels increased significantly in HFrEF-T2DM group compared with HFrEF group (P< 0.001). Correlation analysis showed that serum vWF, NLR, MPVLR were negatively correlated with LVEF (r=-0.510, -0.403, -0.324,P< 0.001), were positively correlated with NT-proBNP (r=0.616, 0.453, 0.343,P< 0.001). ROC curve analysis showed that MPVLR had the highest sensitivity and vWF had the highest specificity in predicting inflammatory injury in HFrEF patients.Conclusion vWF, NLR, and MPVLR have higher activation levels in HFrEF combined with T2DM, which may be the important reference indexes to predict the severity of the disease. -

-
表 1 3组患者的基本临床特征
Table 1. Basic clinical characteristics of the three groups of subjects
例(%), M(P25, P75), X±S 指标 HFrEF-T2DM组(50例) HFrEF组(50例) 对照组(50例) F/H/χ2 P 年龄/岁 66.80±11.301) 63.58±15.791) 57.50±13.54 5.972 0.003 男性 32(64.0) 34(68.0) 27(54.0) 2.207 0.332 BMI/(kg·m-2) 26.04±4.491)2) 23.34±5.07 23.26±3.91 6.136 0.003 HbA1c/% 7.97±1.541)2) 4.69±1.40 4.87±0.95 97.409 < 0.001 FPG/(mmol·L-1) 8.10±3.621)2) 5.48±1.43 4.94±1.10 26.099 < 0.001 TC/(mmol·L-1) 3.61±1.111) 3.86±1.17 4.25±0.94 4.662 0.011 HDL/(mmol·L-1) 0.99(0.82,1.08)1) 1.06(0.85,1.24) 1.17(0.93,1.40) 14.738 0.001 LDL/(mmol·L-1) 2.18(1.33,2.91) 2.32(1.88,3.11) 2.45(2.05,3.15) 5.953 0.051 血清肌酐/(μmol·L-1) 97.66±36.611) 86.26±29.941) 69.55±18.58 11.614 < 0.001 收缩压/mmHg 120(104,135)1) 120(110,140)1) 140(129,166) 24.393 < 0.001 舒张压/mmHg 76.18±11.141) 81.90±18.39 88.08±14.81 7.798 0.001 心率/(次·min-1) 91.26±19.051)2) 78.66±16.61 82.66±12.11 7.919 0.001 NT-proBNP/(pg·mL-1) 4790(2483,8250)1)2) 2331(1727,4875)1) 29(19,41) 106.051 < 0.001 冠心病 38(76.0)2) 24(48.0) 0(0) 8.319 0.004 心房颤动 13(26.0) 17(34.0) 0(0) 0.762 0.383 ACEI/ARB/ARIN 44(88.0) 43(86.0) 0(0) 0.088 0.766 β受体阻滞剂 46(92.0) 45(90.0) 0(0) 0.122 0.727 阿司匹林 34(69.4) 26(53.1) 0(0) 2.751 0.097 CCB 7(14.0) 3(6.0) 0(0) 1.778 0.182 他汀类 45(93.8) 41(82.0) 0(0) 3.147 0.076 LVEDD/mm 61.52±8.321) 63.22±9.061) 47.40±4.44 66.176 < 0.001 LVEF/% 29.48±6.101) 30.54±6.921) 65.72±6.80 490.866 < 0.001 与对照组比较,1)P < 0.05;与HFrEF组比较,2)P < 0.05。 表 2 3组患者血清vWF、NLR、MPVLR表达水平
Table 2. The expression levels of serum vWF, NLR and MPVLR in three groups of patients
M(P25, P75) 指标 HFrEF-T2DM组(50例) HFrEF组(50例) 对照组(50例) F/H/χ2 P vWF/(ng·mL-1) 14.51(13.73,14.92)1)2) 13.22(11.93,14.65)1) 11.87(11.26,12.27) 69.358 < 0.001 NLR 3.69(2.62,5.53)1)2) 2.79(2.06,3.71)1) 1.94(1.31,2.40) 35.176 < 0.001 MPVLR 7.69(6.18,9.36)1)2) 6.32(5.31,8.22)1) 5.07(4.11,7.09) 24.309 < 0.001 与对照组比较,1)P < 0.05;与HFrEF组比较,2)P < 0.05。 表 3 vWF、NLR、MPVLR在HFrEF患者中的预测价值
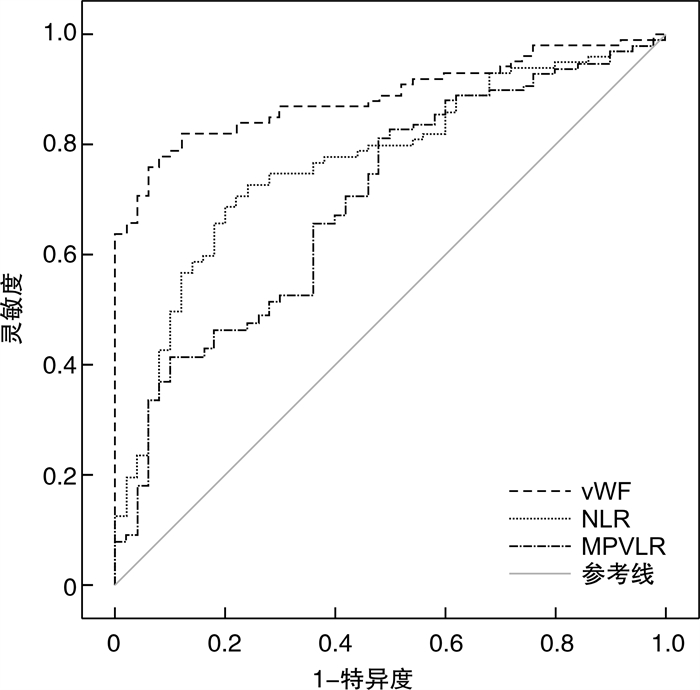
Table 3. Predictive value of vWF, NLR and MPVLR in all HFrEF patients
指标 AUC 95%CI 灵敏度/% 特异度/% 截断值 vWF/(ng·mL-1) 0.888 0.837~0.939 82 70 12.463 NLR 0.770 0.692~0.847 73 49 2.411 MPVLR 0.702 0.615~0.789 89 27 4.711 -
[1] 张婷, 郭文玲. 慢性射血分数降低性心力衰竭治疗的研究进展[J]. 中西医结合心脑血管病杂志, 2019, 17(16): 2458-2461. doi: 10.12102/j.issn.1672-1349.2019.16.016
[2] 马丽萍. 沙库巴曲缬沙坦对糖尿病合并心力衰竭患者的疗效观察[J]. 中国药物与临床, 2021, 21(10): 1703-1705. https://www.cnki.com.cn/Article/CJFDTOTAL-YWLC202110028.htm
[3] 石小溪, 赵宇飞, 田树光, 等. 联合入院时及出院前中性粒细胞/淋巴细胞比值对射血分数降低的心力衰竭患者长期全因死亡的预测价值[J]. 中华医学杂志, 2021, 101(38): 3146-3151. doi: 10.3760/cma.j.cn112137-20210701-01483
[4] Randeria SN, Thomson G, Nell TA, et al. Inflammatory cytokines in type 2 diabetes mellitus as facilitators of hypercoagulation and abnormal clot formation[J]. Cardiovasc Diabetol, 2019, 18(1): 72. doi: 10.1186/s12933-019-0870-9
[5] Hanna A, Frangogiannis NG. Inflammatory Cytokines and Chemokines as Therapeutic Targets in Heart Failure[J]. Cardiovasc Drugs Ther, 2020, 34(6): 849-863. doi: 10.1007/s10557-020-07071-0
[6] Peng X, Wang X, Fan M, et al. Plasma levels of von Willebrand factor in type 2 diabetes patients with and without cardiovascular diseases: A meta-analysis[J]. Diabetes Metab Res Rev, 2020, 36(1): e3193.
[7] 常淑平, 俎小华, 谢泞鲜. 心力衰竭病人vWF、VPO1、NT-proBNP水平与心力衰竭严重程度的相关性分析[J]. 中西医结合心脑血管病杂志, 2019, 17(18): 2873-2875. doi: 10.12102/j.issn.1672-1349.2019.18.043
[8] Heitmar R, Blann AD. Oxygen saturation in retinal vessels and their correlation with endothelial microparticles in diabetes mellitus and/or cardiovascular disease[J]. Microvasc Res, 2022, 142: 104336. doi: 10.1016/j.mvr.2022.104336
[9] Angkananard T, Inthanoo T, Sricholwattana S, et al. The Predictive role of Neutrophil-to-Lymphocyte Ratio(NLR)and Mean Platelet Volume-to-Lymphocyte Ratio(MPVLR)for Cardiovascular Events in Adult Patients with Acute Heart Failure[J]. Mediators Inflamm, 2021, 2021: 6889733.
[10] Hashemi Moghanjoughi P, Neshat S, Rezaei A, et al. Is the Neutrophil-to-Lymphocyte Ratio an Exceptional Indicator for Metabolic Syndrome Disease and Outcomes?[J]. Endocr Pract, 2022, 28(3): 342-348. doi: 10.1016/j.eprac.2021.11.083
[11] Hudzik B, Szkodziński J, Lekston A, et al. Mean platelet volume-to-lymphocyte ratio: a novel marker of poor short-and long-term prognosis in patients with diabetes mellitus and acute myocardial infarction[J]. J Diabetes Complications, 2016, 30(6): 1097-102. doi: 10.1016/j.jdiacomp.2016.04.010
[12] 包丽雯. 射血分数保留心力衰竭与2型糖尿病的研究进展[J]. 复旦学报(医学版), 2020, 47(5): 789-794. doi: 10.3969/j.issn.1672-8467.2020.05.023
[13] 海茹丽妮萨·亚森, 于子翔, 刘芬, 等. 2型糖尿病合并射血分数中间值心力衰竭的内皮功能及预后研究[J]. 中国循证医学杂志, 2021, 21(5): 539-545. https://www.cnki.com.cn/Article/CJFDTOTAL-ZZXZ202105008.htm
[14] 黄丽, 齐洁, 崔建国, 等. 中性粒细胞/淋巴细胞比值与慢性心力衰竭急性发作患者院内死亡的相关性研究[J]. 临床心血管病杂志, 2020, 36(2): 138-142. https://www.cnki.com.cn/Article/CJFDTOTAL-LCXB202002010.htm
[15] Zaccardi F, Rocca B, Pitocco D, et al. Platelet mean volume, distribution width, and count in type 2 diabetes, impaired fasting glucose, and metabolic syndrome: a meta-analysis[J]. Diabetes Metab Res Rev, 2015, 31(4): 402-410. doi: 10.1002/dmrr.2625
[16] 丁绍祥, 周旭东, 高云涛. 左室射血分数与心率比值对老年心力衰竭患者心功能的评估[J]. 中国老年学杂志, 2022, 42(4): 778-781. https://www.cnki.com.cn/Article/CJFDTOTAL-ZLXZ202204004.htm
[17] 田得宽, 苏晓灵, 李卫, 等. 沙库巴曲缬沙坦钠对青海地区射血分数降低的心力衰竭患者心功能及心肌纤维化指标的疗效评价[J]. 临床心血管病杂志, 2022, 38(2): 137-141. https://www.cnki.com.cn/Article/CJFDTOTAL-LCXB202202011.htm
-




 下载:
下载: