The early outcomes of transcatheter valve-in-valve implantation treatment for mitral bioprosthetic valve dysfunction
-
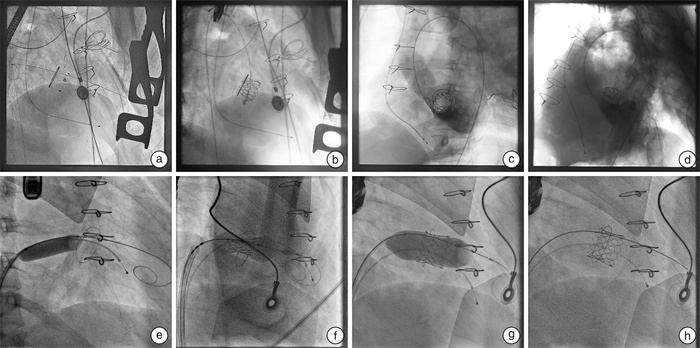
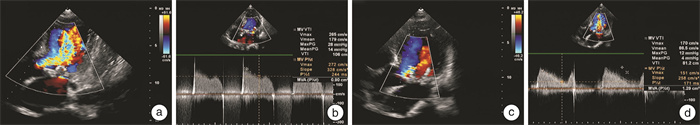
摘要: 目的 总结生物瓣毁损患者行介入二尖瓣瓣中瓣手术的经验和早期效果。方法 回顾性分析2019年1月—2022年3月在郑州大学第一附属医院行介入瓣中瓣手术治疗二尖瓣生物瓣毁损的19例患者的临床资料、手术效果及并发症情况。结果 19例患者中,既往置换Medtronic HancockⅡ瓣膜5例,Edwards Perimount瓣膜1例,佰仁思生物瓣膜1例,St Jude Medical Epic瓣膜12例。瓣膜型号25号10例,27号7例,29号2例。手术于杂交手术室完成,在X线透视及TEE检测下经心尖途径或经股静脉-房间隔途径,将压缩的介入瓣膜在导丝引导下植入二尖瓣生物瓣内。19例患者均成功经心尖入路或经房间隔入路完成介入二尖瓣瓣中瓣植入术。1例术后8 h内发生活动性出血,1例术后随访2年后死亡,其余17例患者无死亡及严重并发症发生。术后3个月完成全部随访,NYHA心功能分级较术前明显改善(P < 0.05),二尖瓣均无反流,峰值流速[(1.81±0.36) m/s vs (2.61±0.49) m/s,P < 0.05]及平均跨瓣压差[(6.1±2.3) mmHg vs(12.5±5.9) mmHg,1 mmHg=0.133 kPa,P < 0.05]明显下降。结论 对于外科手术高风险或禁忌患者,介入瓣中瓣技术治疗二尖瓣生物瓣毁损可获得良好的早期效果。Abstract: Objective To summarize the experience and early outcomes of transcatheter mitral valve-in-valve implantation treatment in patients with bioprosthetic valve dysfunction.Methods The clinical data, surgical results, and complications of 19 patients who received transcatheter mitral valve-in-valve implantation for mitral bioprosthetic valve dysfunction in the First Affiliated Hospital of Zhengzhou University from January 2019 to March 2022 were retrospectively analyzed.Results In terms of the type of the mitral bioprosthetic valve, there were 5 cases of Medtronic Hancock Ⅱ valves, one case of Edwards Perimount valve, one case of BalMedic valve, and 12 cases of St Jude Medical Epic valves. The mitral bioprosthetic size included 25#for 10 cases, 27#for 7 cases, and 29#for 2 cases. The valve-in-valve procedure was completed in the hybrid operating room, and the compressed interventional valve was implanted into the mitral bioprosthetic valve under the guidance of the guide wire through the apical approach or the femoral vein to atrial septal approach under the detection of X-ray fluoroscopy and TEE. All 19 patients completed the interventional mitral valve-in-valve implantation through the apical approach or the atrial septal approach. One patient developed active bleeding within 8 hours after the operation, one patient died after 2 years of follow-up, and the remaining 17 patients had no death or serious complications. All follow-ups were completed 3 months after the operation, NYHA cardiac functional class was significantly improved(P < 0.05), there was no mitral regurgitation after operation, and the mitral peak valve velocity[(1.81±0.36) m/s vs(2.61±0.49) m/s, P < 0.05]and the mitral mean valve pressure gradient[(6.1±2.3) mmHg vs(12.5±5.9) mmHg, 1 mmHg=0.133 kPa, P < 0.05]were significantly decreased.Conclusion For patients with high surgical risk or contraindications, transcatheter mitral valve-in-valve implantation treatment for mitral bioprosthetic valve dysfunction can achieve good early results.
-

-
表 1 二尖瓣生物瓣毁损患者瓣中瓣植入后资料
Table 1. Postoperative data
例, X±S 项目 数值 植入瓣膜途径 心尖途径 18 股静脉途径 1 植入瓣膜类型 佰仁思 13 J-Valve 5 Sapien3 1 植入瓣膜型号 23号 10 25号 6 27号 3 手术时间/min 112.0±44.1 术后拔管时间/h 17.7±21.9 术后ICU监护时间/h 54.8±32.7 术后住院时间/d 10.1±4.3 表 2 瓣中瓣手术前后超声心动图资料比较
Table 2. Comparison of echocardiography three months after surgery
X±S 项目 术前 术后 出院前 t值 P值a) 术后3个月 t值 P值a) 左房内径/mm 52.63±9.67 47.00±9.25 5.244 < 0.001 45.90±10.10 6.295 < 0.001 左室舒张内径/mm 49.16±5.57 45.00±5.70 4.027 0.001 44.32±4.60 4.076 0.001 肺动脉压力/mmHg 49.42±20.20 36.89±11.14 3.601 0.002 41.16±25.62 1.755 0.096 二尖瓣峰值流速/(m·s-1) 2.61±0.49 1.84±0.43 4.704 < 0.001 1.81±0.36 5.467 < 0.001 二尖瓣平均跨瓣压差/mmHg 12.5±5.9 6.6±2.9 3.734 0.002 6.1±2.3 4.296 < 0.001 左室射血分数/% 62.89±3.81 63.05±2.46 -0.217 0.830 61.53±4.49 1.127 0.275 a)与术前比较。 表 3 瓣中瓣手术前后瓣膜反流情况及心功能指标比较
Table 3. Comparison of postoperative valve reflux and cardiac function
例(%) 项目 术前 术后 出院前 Z值 P值 术后3个月 Z值 P值 二尖瓣反流分级 -3.611 < 0.001 -3.611 < 0.001 无反流 3(16) 16(84) 19(100) 轻度(反流面积 < 4 cm2) 1(5) 3(16) 0(0) 中度(反流面积4~8 cm2) 6(32) 0(0) 0(0) 重度(反流面积>8 cm2) 9(47) 0(0) 0(0) NYHA心功能分级 -4.021 < 0.001 -3.934 < 0.001 Ⅰ 0(0) 1(5) 2(10) Ⅱ 0(0) 13(69) 14(74) Ⅲ 10(53) 5(26) 3(16) Ⅳ 9(47) 0(0) 0(0) -
[1] 孟旭, 白涛. 5066例瓣膜手术的围术期临床回顾[J]. 中华胸心血管外科杂志, 2007, 23(1): 11-13. https://cpfd.cnki.com.cn/Article/CPFDTOTAL-ZHYX200504002060.htm
[2] 张海波, 孟旭, 王胜洵, 等. 二尖瓣生物瓣毁损的J-Valve介入瓣中瓣技术短期随访临床经验[J]. 华西医学, 2020, 35(9): 1108-1112. https://www.cnki.com.cn/Article/CJFDTOTAL-HXYX202009016.htm
[3] Barbanti M, Costa G, Zappulla P, et al. Incidence of long-term structural valve dysfunction and bioprosthetic valve failure after transcatheter aortic valve replacement[J]. J Am Heart Assoc, 2018, 7(15): e008440. doi: 10.1161/JAHA.117.008440
[4] Leontyev S, Borger MA, Davierwala P, et al. Redo aortic valve surgery: early and late outcomes[J]. Ann Thorac Surg, 2011, 91(4): 1120-1126. doi: 10.1016/j.athoracsur.2010.12.053
[5] Mehaffey HJ, Hawkins RB, Schubert S, et al. Contemporary outcomes in reoperative mitral valve surgery[J]. Heart, 2018, 104(8): 652-656. doi: 10.1136/heartjnl-2017-312047
[6] Cribier A, Eltchaninoff H, Bash A, et al. Percutaneous transcatheter implantation of an aortic valve prosthesis for calcific aortic stenosis: first human case description[J]. Circulation, 2002, 106(24): 3006-3008. doi: 10.1161/01.CIR.0000047200.36165.B8
[7] 魏培坚, 刘健, 谢年谨, 等. 主动脉瓣及二尖瓣双瓣置换术后二尖瓣生物瓣衰败的经心尖经导管瓣中瓣治疗[J]. 中国胸心血管外科临床杂志, 2021, 28(8): 901-907. https://www.cnki.com.cn/Article/CJFDTOTAL-ZXYX202108006.htm
[8] 中国结构性心脏病介入治疗进展报告2020[J]. 中国循环杂志, 2021, 36(9): 833-840.
[9] den Heijer P. Transcatheter aortic valve implantation: first choice for aortic stenosis?[J]. Neth Heart J, 2020, 28(5): 227-228. doi: 10.1007/s12471-020-01419-9
[10] Carroll JD, Mack MJ, Vemulapalli S, et al. STS-ACC TVT Registry of transcatheter aortic valve replacement[J]. J Am Coll Cardiol, 2020, 76(21): 2492-2516. doi: 10.1016/j.jacc.2020.09.595
[11] 张海波, 孟旭. 经导管主动脉瓣置入手术的历史与现状[J]. 中国心血管病研究, 2020, 18(4): 289-294. https://www.cnki.com.cn/Article/CJFDTOTAL-XXGZ202004001.htm
[12] Shreenivas S, Kaneko T, Tang G. Predicting the future of TAVR: an obituary to open aortic valve replacement?[J]. Curr Opin Cardiol, 2019, 34(2): 112-123. doi: 10.1097/HCO.0000000000000609
[13] Jones JM, O'Kane H, Gladstone DJ, et al. Repeat heart valve surgery: risk factors for operative mortality[J]. J Thorac Cardiovasc Surg, 2001, 122(5): 913-918. doi: 10.1067/mtc.2001.116470
[14] Webb JG, Wood DA, Ye J, et al. Transcatheter valve-in-valve implantation for failed bioprosthetic heart valves[J]. Circulation, 2010, 121(16): 1848-1857. doi: 10.1161/CIRCULATIONAHA.109.924613
[15] Cheung A, Webb JG, Wong DR, et al. Transapical transcatheter mitral valve-in-valve implantation in a human[J]. Ann Thorac Surg, 2009, 87(3): e18-e20. doi: 10.1016/j.athoracsur.2008.10.016
[16] Cerillo AG, Gasbarri T, Celi S, et al. Transapical transcatheter valve-in-valve implantation for failed mitral bioprostheses: gradient, symptoms, and functional status in 18 high-risk patients up to 5 years[J]. Ann Thorac Surg, 2016, 102(4): 1289-1295. doi: 10.1016/j.athoracsur.2016.03.051
[17] 张海波, 孟旭, 王胜洵, 等. 经导管二尖瓣生物瓣毁损的瓣中瓣治疗技术[J]. 中华胸心血管外科杂志, 2019, 35(6): 331-333. https://www.cnki.com.cn/Article/CJFDTOTAL-WZYX202208012.htm
[18] Hsiung MC, Yin WH, Lee YT, et al. Effects of transapical transcatheter mitral valve implantation[J]. Front Cardiovasc Med, 2021, 8: 633369.
[19] Cheung A, Al-Lawati A. Transcatheter mitral valve-in-valve implantation: current experience and review of literature[J]. Curr Opin Cardiol, 2013, 28(2): 181-186.
[20] Seiffert M, Conradi L, Baldus S, et al. Transcatheter mitral valve-in-valve implantation in patients with degenerated bioprostheses[J]. JACC Cardiovasc Interv, 2012, 5(3): 341-349.
[21] Wilbring M, Alexiou K, Tugtekin SM, et al. Transapical transcatheter valve-in-valve implantation for deteriorated mitral valve bioprostheses[J]. Ann Thorac Surg, 2013, 95(1): 111-117.
[22] 谢旭晶, 李力夫, 黄焕雷, 等. 经心尖二尖瓣瓣中瓣手术的早期结果[J]. 中华胸心血管外科杂志, 2021, 37(10): 600-605.
-




 下载:
下载: