Fragmented QRS complex and nonresponse to cardiac resynchronization therapy: a meta analysis
-
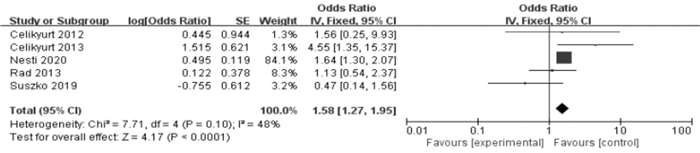
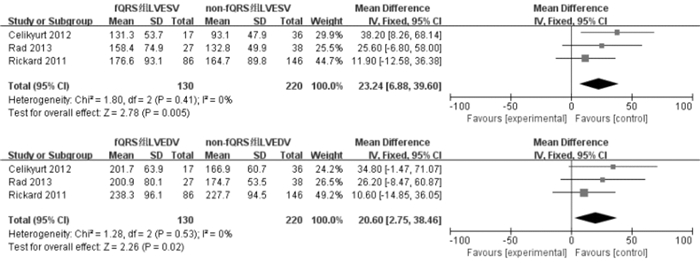
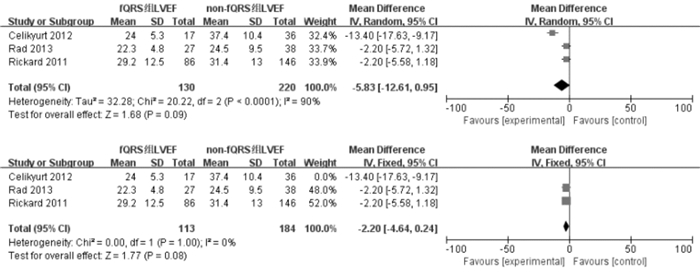
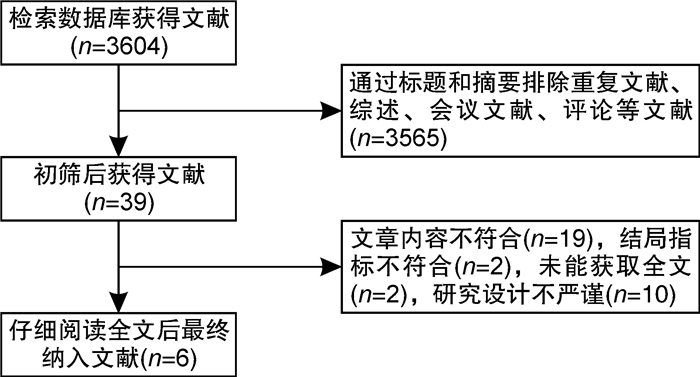
摘要: 目的 评估碎裂QRS波(fragmented QRS,fQRS)与心力衰竭患者接受心脏再同步化治疗(CRT)后无反应性之间的关联。方法 在PubMed、The Cochrane Library、Web of science、EMbase、中国知网、万方、维普网和中国生物医学文献服务系统数据库中全面检索从建库至2022年10月评估fQRS与CRT反应性的相关文献,由2名研究者独立筛选、提取文献,对纳入研究进行质量评价。RevMan 5.4和STATA/MP 14软件行荟萃分析,并且对研究结果进行发表偏倚分析。结果 总纳入6篇研究,纳入研究之间异质性无统计学意义,荟萃分析结果显示CRT治疗前fQRS的存在与CRT治疗无反应性相关(OR=1.58,95%CI1.27~1.95,P < 0.001)。此外,针对fQRS的存在对CRT植入后左室收缩末期容积和左室舒张末期容积改善程度进行亚组分析,合并效应量分别为(MD=23.24,95%CI6.88~39.60,P=0.005,I2=0%)和(MD=20.60,95%CI2.75~38.46,P=0.02,I2=0%)。结论 fQRS与CRT无反应相关。Abstract: Objective To assess whether fragmented QRS(fQRS) is an predictor of nonresponse to cardiac resynchronization therapy(CRT) in patients with heart failure.Methods Two investigators independently performed a comprehensive search on topics that assesses fQRS and its association with nonresponse to CRT and remodeling up until May 2022. Meta-analyses were performed with RevMan 5.4 and STATA/MP 14, and publication bias analyses were performed on the findings.Results In a total of 6 studies, the results of the meta-analysis showed that the presence of fQRS was related to non-response to CRT(OR=1.58, 95%CI, 1.27-1.95, P < 0.001). In addition, the results of subgroup analysis showed that the presence of fQRS also associated with left ventricular end systolic volume(LVESV) and left ventricular end diastolic volume(LVEDV) reduction after CRT, and the pooled effect amounts were(MD=23.24, 95%CI6.88-39.60, P=0.005, I2=0%)and(MD=20.60, 95%CI2.75-38.46, P=0.02, I2=0%) respectively.Conclusion Fragmented QRS is associated with nonresponse to cardiac resynchronization therapy and ventricular remodeling after CRT.
-
Key words:
- fragmented QRS /
- cardiac resynchronization therapy /
- meta analysis
-

-
表 1 6篇fQRS与CRT反应性相关研究的基本特征
Table 1. Basic characteristics of 6 studies on the correlation between fQRS and CRT reactivity
研究 研究设计 患者特征 总人数/例 fQRS总人数/例 QRS时限/ms QRS时限/ms(fQRS/non-fQRS) LBBB/% 缺血性心肌病/% 随访时间/月 CRT反应性标准 NOS评分/分 Celikyurt,2012 前瞻性队列研究 纽约分级Ⅲ~Ⅳ级,LVEF≤35%,QRS宽度≥120 ms,全部患者有LBBB 53 17 - 143±13/138±13 100 44 6 LVESV减少≥15% 8 Rad,2013 前瞻性队列研究 纽约分级Ⅲ~Ⅳ级,LVEF≤35%,QRS宽度≥120 ms 65 27 - 142.6±13.5/137.4±11.8 - - 3~6 LVESV减少≥15% 8 Celikyurt,2013 病例对照研究 纽约分级Ⅲ~Ⅳ级,LVEF≤35%,QRS宽度≥120 ms,全部患者有LBBB 105 48 146±18 - 100 39 6 LVESV减少≥15% 7 Nesti,2020 病例对照研究 纽约分级Ⅱ~Ⅲ级,LVEF≤35%,QRS宽度≥120 ms,全部患者有LBBB,植入CRTD 178 74 161±18 - 100 36 6 LVESV减少≥15%或LVEF增多≥10% 6 Suszko,2019 病例对照研究 纽约分级Ⅱ~Ⅳ级,LVEF≤35%,QRS≥120 ms伴LBBB或无LBBB伴QRS≥150 ms,植入CRTD 47 25 173±32 - 87 34 6 LVEF比基线水平增高 > 5% 6 Rickard,2011 回顾性队列研究 纽约分级Ⅱ~Ⅳ级,LVEF≤40% 232 86 161.8±29.5 174.5±27.2/158.3±29.2 43 52 11.6±9.0 LVEF、LVEDV、LVESV的显著改变 7 注:LBBB表示左束支传导阻滞;-表示未能获取的数据。 -
[1] 孔洪. 重视慢性心力衰竭恶化的患者管理[J]. 临床心血管病杂志, 2021, 37(4): 289-292. doi: 10.13201/j.issn.1001-1439.2021.04.001
[2] Leyva F, Nisam S, Auricchio A. 20 Years of Cardiac Resynchronization Therapy[J]. J Am Coll Cardiol, 2014, 64(10): 1047-1058. doi: 10.1016/j.jacc.2014.06.1178
[3] Chatterjee S, Changawala N. Fragmented QRS complex: a novel marker of cardiovascular disease[J]. Clinical Cardiology, 2010, 33(2): 68-71. doi: 10.1002/clc.20709
[4] Basaran Y, Tigen K, Karaahmet T, et al. Fragmented QRS complexes are associated with cardiac fibrosis and significant intraventricular systolic dyssynchrony in nonischemic dilated cardiomyopathy patients with a narrow QRS interval[J]. Echocardiography, 2011, 28(1): 62-68. doi: 10.1111/j.1540-8175.2010.01242.x
[5] Das MK, Zipes DP. Fragmented QRS: a predictor of mortality and sudden cardiac death[J]. Heart Rhythm, 2009, 6(3): S8-14. doi: 10.1016/j.hrthm.2008.10.019
[6] Das MK, Khan B, Jacob S, et al. Significance of a fragmented QRS complex versus a Q wave in patients with coronary artery disease[J]. Circulation, 2006, 113(21): 2495-2501. doi: 10.1161/CIRCULATIONAHA.105.595892
[7] Sha J, Zhang S, Tang M, et al. Fragmented QRS is associated with all-cause mortality and ventricular arrhythmias in patient with idiopathic dilated cardiomyopathy[J]. Ann Noninvasive Electrocardiol, 2011, 16(3): 270-275. doi: 10.1111/j.1542-474X.2011.00442.x
[8] Sinha SK, Bhagat K, Asif M, et al. Fragmented QRS as a marker of electrical dyssynchrony to predict inter-ventricular conduction defect by subsequent echocardiographic assessment in symptomatic patients of non-ischemic dilated cardiomyopathy[J]. Cardiol Res, 2016, 7(4): 140-145. doi: 10.14740/cr495w
[9] Tigen K, Karaahmet T, Gurel E, et al. The utility of fragmented qrs complexes to predict significant intraventricular dyssynchrony in nonischemic dilated cardiomyopathy patients with a narrow QRS Interval[J/OL]. Can J Cardiol, 2009, 25(9): 517-522.
[10] Heidenreich PA, Bozkurt B, Aguilar D, et al. 2022 AHA/ACC/HFSA Guideline for the Management of Heart Failure: A Report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines[J]. Circulation, 2022, 145(18): e895-e1032.
[11] Celikyurt U, Agacdiken A, Sahin T, et al. Relationship between fragmented QRS and response to cardiac resynchronization therapy[J]. J Interv Card Electrophysiol, 2012, 35(3): 337-342. doi: 10.1007/s10840-012-9715-0
[12] Celikyurt U, Agacdiken A, Sahin T, et al. Number of leads with fragmented QRS predicts response to cardiac resynchronization therapy[J]. Clin Cardiol, 2013, 36(1): 36-39. doi: 10.1002/clc.22061
[13] Assadian Rad M, Tabarzan Baboli N, Barzigar A, et al. The Role of the Fragmented QRS complexes on a routine 12-lead ECG in predicting non-responsiveness to cardiac resynchronization Therapy[J]. Anatol J Cardiol, 2015, 15(3): 204-208. doi: 10.5152/akd.2014.5307
[14] Rickard J, Zardkoohi O, Popovic Z, et al. QRS fragmentation is not associated with poor response to cardiac resynchronization therapy[J]. Ann Noninvasive Electrocardiol, 2011, 16(2): 165-171. doi: 10.1111/j.1542-474X.2011.00424.x
[15] Suszko AM, Nayyar S, Porta-Sanchez A, et al. Quantification of abnormal QRS peaks predicts response to cardiac resynchronization therapy and tracks structural remodeling[J]. PLoS ONE, 2019, 14(6): 1-17.
[16] Nesti M, Perini AP, Bani R, et al. Myocardial scar on surface ECG: selvester score, but not fragmentation, predicts response to CRT[J]. Cardiol Res Pract, 2020, 2020: 2036545.
[17] Varriale P, Chryssos BE. The RSR'Complex not related to right bundle branch block: diagnostic value as a sign of myocardial infarction scar[J]. Am Heart J, 1992, 123(2): 369-376. doi: 10.1016/0002-8703(92)90648-F
[18] Das MK, Maskoun W, Shen C, et al. Fragmented QRS on twelve-lead electrocardiogram predicts arrhythmic events in patients with ischemic and nonischemic cardiomyopathy[J]. Heart Rhythm, 2010, 7(1): 74-80. doi: 10.1016/j.hrthm.2009.09.065
[19] Bax JJ, Bleeker GB, Marwick TH, et al. Left ventricular dyssynchrony predicts response and prognosis after cardiac resynchronization therapy[J]. J Am Coll Cardiol, 2004, 44(9): 1834-1840. doi: 10.1016/j.jacc.2004.08.016
[20] Pranata R, Yonas E, Vania R, et al. Fragmented QRS is associated with intraventricular dyssynchrony and independently predicts nonresponse to cardiac resynchronization therapy-systematic review and meta-analysis[J]. Ann Noninvasive Electrocardiol, 2020, 25(4): e12750.
[21] Hu YR, Hua W, Yang SW, et al. Predictors of non-response to cardiac resynchronization therapy implantation in patients with class i indications: the markedly dilated left ventricular end-diastolic dimension and the presence of fragmented QRS[J]. J Geriatr Cardiol, 2019, 16(7): 514-521.
[22] Vandenberk B, Robyns T, Goovaerts G, et al. Inter-and intra-observer variability of visual fragmented QRS scoring in ischemic and non-ischemic cardiomyopathy[J]. J Electrocardiol, 2018, 51(3): 549-554. doi: 10.1016/j.jelectrocard.2017.12.002
[23] 高蓉蓉, 徐芳, 祝绪, 等. 全血细胞衍生的炎症标志物对急性心力衰竭患者的长期预后价值[J]. 临床心血管病杂志, 2022, 38(12): 980-987.
-




 下载:
下载: