Relationship of serum MOTS-c and sLRP-1 levels with the severity and prognosis of patients with acute coronary syndrome
-
摘要: 目的 测定急性冠状动脉综合征(ACS)患者血清线粒体衍生肽(MOTS-c)和可溶性低密度脂蛋白受体相关蛋白-1(sLRP-1)水平,探究其与冠状动脉(冠脉)病变严重程度及预后的相关性。方法 选取行冠脉造影(CAG)患者240例,其中不稳定心绞痛患者109例(UAP组),急性心肌梗死患者79例(AMI组),CAG正常者52例(对照组)。收集患者一般资料并测定血清MOTS-c、sLRP-1水平。根据CAG结果评估冠脉病变支数和病变程度,记录患者平均随访10个月中的主要不良心血管事件(MACEs)发生情况。结果 与对照组比较,UAP组和AMI组患者血清MOTS-c水平均明显降低,sLRP-1水平明显升高,且AMI组患者血清MOTS-c水平显著低于UAP组,sLRP-1水平显著高于UAP组,均差异有统计学意义(均P < 0.05)。随着病变程度加重,血清MOTS-c水平逐渐降低,sLRP-1水平逐渐升高(P < 0.05)。单支病变组、双支病变组、多支病变组患者血清MOTS-c水平依次降低,sLRP-1水平依次升高(P < 0.05)。Spearman分析显示,ACS患者血清MOTS-c水平与MACEs呈负相关(r=-0.381,P < 0.001),sLRP-1水平与MACEs呈正相关(r=0.338,P < 0.001)。血清MOTS-c、sLRP-1水平对ACS患者的预后具有预测价值,曲线下面积分别为0.762、0.732,灵敏度分别为86.0%、83.7%,特异度分别为64.8%、67.6%。结论 血清MOTS-c水平降低、sLRP-1水平升高与ACS患者病情严重程度及预后不良相关。Abstract: Objective To measure the serum levels of MOTS-c and sLRP-1 in patients with acute coronary syndrome(ACS) and to investigate their relationship with the severity of coronary lesions and prognosis.Methods Two hundred and forty patients who underwent coronary angiography(CAG) were selected and divided into unstable angina group(n=109), acute myocardial infarction group(n=79), and control group(n=52). General data were collected and serum MOTS-c and sLRP-1 levels were measured. The number of coronary lesion branches and the extent of lesions were assessed according to the CAG results, and the occurrence of major adverse cardiovascular events(MACEs) was recorded during the 10-month follow-up.Results Compared with the control group, serum MOTS-c levels were significantly lower and sLRP-1 levels were significantly higher in both the UAP and AMI groups, and serum MOTS-c levels were significantly lower and sLRP-1 levels were significantly higher in the AMI group than those in the UAP group(all P < 0.05). Serum MOTS-c levels gradually decreased and sLRP-1 levels gradually increased with the increase of lesion degree(P < 0.05). The serum MOTS-c levels decreased and sLRP-1 levels increased in the single-branch lesion group, the double-branch lesion group, and the multi-branch lesion group in that order(P < 0.05). Spearman analysis showed that the serum MOTS-c level in ACS patients was negatively correlated with MACEs(r=-0.381, P < 0.001), and the sLRP-1 level was positively correlated with MACEs(r=0.338, P < 0.001). Serum MOTS-c and sLRP-1 levels had a predictive value for the prognosis of ACS patients, whose areas under the curve were 0.762 and 0.732, with sensitivity of 86.0% and 83.7%, and specificity of 64.8% and 67.6%, respectively.Conclusion Decreased serum MOTS-c levels and increased sLRP-1 levels are associated with severity and poor prognosis in patients with ACS.
-
Key words:
- acute coronary syndrome /
- MOTS-c /
- sLRP-1 /
- major adverse cardiac events
-

-
表 1 基线资料及实验室指标比较
Table 1. Comparison of baseline data and laboratory indicators
例(%), X±S, M(P25, P75) 项目 对照组(52例) UAP组(109例) AMI组(79例) P 男性 12(23.1) 56(51.4)1) 56(70.9)1)2) < 0.001 年龄/岁 59.77±7.66 65.39±7.581) 63.30±9.811) 0.002 BMI/(kg/m2) 24.29±3.37 25.60±3.481) 25.65±2.761) 0.033 收缩压/mmHg 129.92±17.73 137.07±16.02 136.29±22.79 0.059 舒张压/mmHg 74.42±10.71 76.13±10.31 79.96±13.051) 0.014 饮酒 9(17.3) 31(28.4) 36(45.6)1)2) 0.002 吸烟 10(19.2) 40(36.7)1) 48(60.8)1)2) < 0.001 高血压 29(55.8) 73(67.0) 58(73.4) 0.111 糖尿病 5(9.6) 35(32.1)1) 42(53.2)1)2) < 0.001 冠心病家族史 13(25.0) 21(19.3) 12(15.2) 0.377 TC/(mmol/L) 4.56±0.85 4.54±1.31 4.82±1.18 0.250 TG/(mmol/L) 1.38(0.85,1.73) 1.56(0.98,1.92) 1.93(1.18,2.04)1)2) 0.007 HDL-C/(mmol/L) 1.29±0.36 1.22±0.31 1.04±0.231)2) < 0.001 LDL-C/(mmol/L) 2.90±0.72 2.94±1.08 3.30±1.03 0.057 FBG/(mmol/L) 5.77(5.06,6.06) 6.15(5.17,6.45) 7.42(5.88,7.95)1)2) < 0.001 肌酐/(μmol/L) 59.40±13.64 70.71±16.261) 72.54±21.141) < 0.001 LVEF/% 59.88(59.00,61.00) 58.57(58.00,60.00)1) 54.47(55.00,58.00)1)2) < 0.001 Gensini积分 28.98±27.02 57.92±34.702) < 0.001 GRACE评分 113.32±20.81 144.51±35.172) < 0.001 MOTS-c/(ng/mL) 192.86±39.05 142.01±36.921) 106.39±28.971)2) < 0.001 sLRP-1/(ng/mL) 169.90±43.94 284.01±58.891) 348.36±40.801)2) < 0.001 与对照组比较,1)P < 0.05;与UAP组比较,2)P < 0.05。 表 2 不同冠脉病变程度ACS患者血清MOTS-c、sLRP-1水平比较
Table 2. Comparison of serum MOTS-c and sLRP-1 levels in ACS patients with different degrees of coronary artery lesions
ng/mL, X±S 组别 MOTS-c sLRP-1 轻度狭窄组(64例) 145.82±37.00 277.86±56.47 中度狭窄组(61例) 128.05±37.281) 313.30±60.831) 高度狭窄组(63例) 107.00±29.301)2) 342.58±47.131)2) F 19.90 22.02 P < 0.001 < 0.001 与轻度狭窄组比较,1)P < 0.05;与中度狭窄组比较,2)P < 0.05。 表 3 不同病变支数ACS患者血清MOTS-c、sLRP-1水平比较
Table 3. Comparison of serum MOTS-c and sLRP-1 levels in ACS patients according to the number of diseased vessels
ng/mL, X±S 组别 MOTS-c sLRP-1 单支病变组(35例) 157.67±44.80 276.28±64.79 双支病变组(59例) 129.51±29.571) 292.98±51.43 多支病变组(94例) 114.09±32.271)2) 335.34±54.961)2) F 20.41 18.76 P < 0.001 < 0.001 与单支病变组比较,1)P < 0.05;与双支病变组比较,2)P < 0.05。 表 4 血清MOTS-c、sLRP-1水平对ACS患者发生MACEs的预测价值
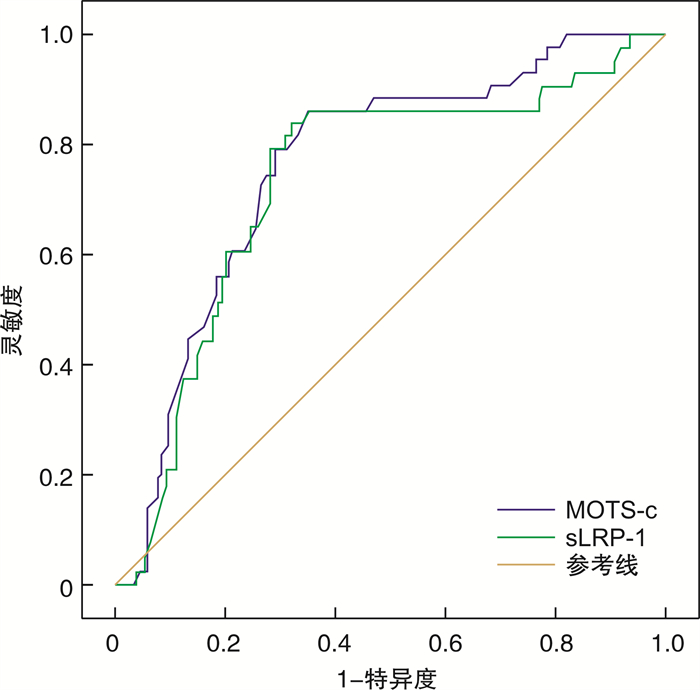
Table 4. Predictive value of serum MOTS-c and sLRP-1 levels on the occurrence of MACEs in ACS patients
项目 AUC(95%CI) 约登指数 截断值 灵敏度/% 特异度/% P MOTS-c 0.762(0.684~0.839) 0.508 120.00 ng/mL 86.0 64.8 < 0.001 sLRP-1 0.732(0.644~0.820) 0.513 339.51 ng/mL 83.7 67.6 < 0.001 -
[1] 《中国心血管健康与疾病报告2021》编写组. 《中国心血管健康与疾病报告2021》要点解读[J]. 中国心血管杂志, 2022, 27(4): 305-318. https://www.cnki.com.cn/Article/CJFDTOTAL-XIXG202204001.htm
[2] Bergmark BA, Mathenge N, Merlini PA, et al. Acute coronary syndromes[J]. Lancet, 2022, 399(10332): 1347-1358. doi: 10.1016/S0140-6736(21)02391-6
[3] 郑淑苹, 罗超迪, 王萍, 等. ACS患者血浆纤维蛋白原与冠状动脉病变严重程度的关系[J]. 临床心血管病杂志, 2021, 37(7): 625-631. doi: 10.13201/j.issn.1001-1439.2021.07.008
[4] Dabravolski SA, Nikiforov NG, Starodubova AV, et al. The Role of Mitochondria-Derived Peptides in Cardiovascular Diseases and Their Potential as Therapeutic Targets[J]. Int J Mol Sci, 2021, 22(16): 8770. doi: 10.3390/ijms22168770
[5] Wan W, Zhang L, Lin Y, et al. Mitochondria-derived peptide MOTS-c: effects and mechanisms related to stress, metabolism and aging[J]. J Transl Med, 2023, 21(1): 36. doi: 10.1186/s12967-023-03885-2
[6] Li H, Ren K, Jiang T, et al. MOTS-c attenuates endothelial dysfunction via suppressing the MAPK/NF-κB pathway[J]. Int J Cardiol, 2018, 268: 40. doi: 10.1016/j.ijcard.2018.03.031
[7] Wei M, Gan L, Liu Z, et al. Mitochondrial-Derived Peptide MOTS-c Attenuates Vascular Calcification and Secondary Myocardial Remodeling via Adenosine Monophosphate-Activated Protein Kinase Signaling Pathway[J]. Cardiorenal Med, 2020, 10(1): 42-50. doi: 10.1159/000503224
[8] Meszaros M, Kunos L, Tarnoki AD, et al. The Role of Soluble Low-Density Lipoprotein Receptor-Related Protein-1 in Obstructive Sleep Apnoea[J]. J Clin Med, 2021, 10(7): 1494. doi: 10.3390/jcm10071494
[9] Actis Dato V, Chiabrando GA. The Role of Low-Density Lipoprotein Receptor-Related Protein 1 in Lipid Metabolism, Glucose Homeostasis and Inflammation[J]. Int J Mol Sci, 2018, 19(6): 1780. doi: 10.3390/ijms19061780
[10] Xian X, Ding Y, Dieckmann M, et al. LRP1 integrates murine macrophage cholesterol homeostasis and inflammatory responses in atherosclerosis[J]. Elife, 2017, 6: e29292. doi: 10.7554/eLife.29292
[11] Mineo C. Lipoprotein receptor signalling in atherosclerosis[J]. Cardiovasc Res, 2020, 116(7): 1254-1274. doi: 10.1093/cvr/cvz338
[12] 张新超, 于学忠, 陈凤英, 等. 急性冠脉综合征急诊快速诊治指南(2019)[J]. 临床急诊杂志, 2019, 20(4): 253-262. https://www.cnki.com.cn/Article/CJFDTOTAL-ZZLC201904001.htm
[13] 钱少环, 李妙男, 姚卓亚, 等. 血清FGF21、CHOP水平与急性冠状动脉综合征及临床预后之间的相关性[J]. 临床心血管病杂志, 2022, 38(10): 790-795. https://lcxxg.whuhzzs.com/article/doi/10.13201/j.issn.1001-1439.2022.10.007
[14] 魏宇淼. 急性心肌梗死并发心源性休克的当代治疗策略及技术[J]. 临床心血管病杂志, 2021, 37(7): 591-594. doi: 10.13201/j.issn.1001-1439.2021.07.001
[15] Miller B, Kim SJ, Kumagai H, et al. Peptides derived from small mitochondrial open reading frames: Genomic, biological, and therapeutic implications[J]. Exp Cell Res, 2020, 393(2): 112056. doi: 10.1016/j.yexcr.2020.112056
[16] Qin Q, Delrio S, Wan J, et al. Downregulation of circulating MOTS-c levels in patients with coronary endothelial dysfunction[J]. Int J Cardiol, 2018, 254: 23-27. doi: 10.1016/j.ijcard.2017.12.001
[17] Benayoun BA, Lee C. MOTS-c: A Mitochondrial-Encoded Regulator of the Nucleus[J]. Bioessays, 2019, 41(9): e1900046. doi: 10.1002/bies.201900046
[18] Yamamoto K, Santamaria S, Botkjaer KA, et al. Inhibition of Shedding of Low-Density Lipoprotein Receptor-Related Protein 1 Reverses Cartilage Matrix Degradation in Osteoarthritis[J]. Arthritis Rheumatol, 2017, 69(6): 1246-1256. doi: 10.1002/art.40080
[19] 田雅楠, 宋海玖, 丁振江, 等. 血浆可溶性低密度脂蛋白受体相关蛋白1对急性冠状动脉综合征患者预后的预测价值[J]. 中国心血管杂志, 2021, 26(3): 237-241. https://www.cnki.com.cn/Article/CJFDTOTAL-XIXG202103008.htm
[20] Brifault C, Gilder AS, Laudati E, et al. Shedding of membrane-associated LDL receptor-related protein-1 from microglia amplifies and sustains neuroinflammation[J]. J Biol Chem, 2017, 292(45): 18699-18712.
-




 下载:
下载: