Efficacy of empagliflozin in type 2 diabetes mellitus patients with sepsis and acute heart failure for 1 years
-
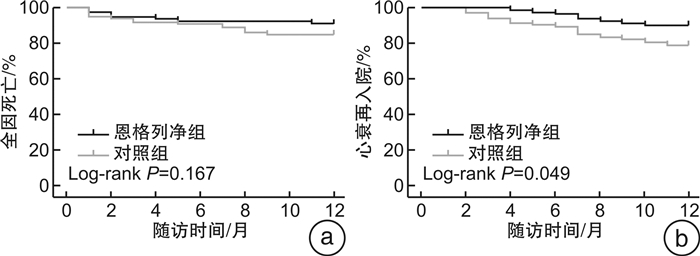
摘要: 目的 探讨恩格列净在脓毒症合并急性心力衰竭(心衰)的2型糖尿病患者中应用的疗效。方法 纳入脓毒症合并急性心力衰竭的糖尿病患者共180例,按不同治疗方式分为恩格列净组(79例)和对照组(101例),比较2组患者12个月全因死亡及心衰再入院的发生率。应用Kaplan-Meier(K-M)法绘制生存曲线,应用Cox回归分析再入院的危险因素。结果 2组患者12个月全因死亡率差异无统计学意义。K-M曲线显示恩格列净组12个月时心衰再入院率显著低于对照组(P=0.049)。多因素Cox回归分析显示恩格列净是心衰再入院的独立保护因素。结论 脓毒症合并急性心衰的2型糖尿病患者应用恩格列净可以显著降低患者12个月心衰再入院率。Abstract: Objective To explore the effect of empagliflozin on the type 2 diabetes mellitus patients with sepsis and acute heart failure.Methods The 180 patients with sepsis and acute heart failure were divided into empagliflozin group with 79 cases and control group with 101 cases according to different treatment methods. The incidence of 12-month all-cause death and rehospitalization with heart failure were compared between the two groups. The survival curve was drawn by Kaplan-Meier(K-M) method. The risk factors of readmission were analyzed by Cox regression.Results There was no significant difference in 12-month all-cause mortality between the two groups. K-M curve showed that the rehospitalization rate of heart failure at 12 months in the empagliflozin group was significantly lower than that in the control group(P=0.049). Multivariate Cox regression analysis showed that empagliflozin was an independent protective factor for rehospitalization of heart failure.Conclusion Empagliflozin can significantly reduce the rehospitalization rate of heart failure in 12 months in type 2 diabetic patients with sepsis and acute heart failure.
-
Key words:
- sepsis /
- acute heart failure /
- type 2 diabetes mellitus /
- empagliflozin
-

-
表 1 恩格列净组和对照组患者基本情况比较
Table 1. Patient characteristics of empagliflozin group and control group
例(%), M(P25, P75), X±S 项目 恩格列净组(79例) 对照组(101例) t/χ2 P 年龄/岁 69.4±10.6 68.7±10.1 0.447 0.656 BMI/(kg·m-2) 24.9±3.9 25.8±3.9 -1.465 0.145 男性 42(53.2) 48(47.5) 0.564 0.453 高血压 56(70.9) 72(71.3) 0.003 0.953 冠心病 25(31.6) 35(34.7) 0.180 0.671 缺血性心脏病 14(17.7) 16(15.8) 0.113 0.737 慢性心功能不全 30(38.0) 44(43.6) 0.572 0.449 慢性肾功能不全 16(20.3) 27(26.7) 1.024 0.312 慢性阻塞性肺疾病 18(22.8) 27(26.7) 0.368 0.544 贫血 14(17.7) 25(24.8) 1.291 0.256 吸烟 32(40.5) 37(37.0) 0.229 0.632 APACHEⅡ评分/分 18(15,21) 17(14.5,20) -1.362 0.173 SOFA评分/分 15(11,19) 14(10,18) -1.223 0.221 糖化血红蛋白/% 8.2±0.5 8.1±0.7 1.059 0.291 白细胞/(×109·L-1) 17.8±3.6 17.3±3.9 0.957 0.340 中性粒细胞比值/% 85.1±3.0 85.4±3.4 -0.680 0.497 降钙素原/(ng·mL-1) 5.7±2.3 5.1±2.2 1.517 0.131 血红蛋白/(g·L-1) 116.1±13.0 120.7±15.0 -2.159 0.032 血小板/(×109·L-1) 129.6±38.5 132.9±33.9 -0.623 0.534 血肌酐/(μmol·L-1) 106(83,125) 106(93,128) -1.195 0.232 NT-proBNP/(pg·mL-1) 5648.5±462.4 5524.9±486.5 1.728 0.086 LVEDD/mm 55.0±7.5 54.1±5.4 0.946 0.345 LVEF/% 46.9±12.1 48.9±9.3 -1.228 0.221 机械通气 20(25.3) 19(18.8) 1.105 0.293 ICU/d 7.0±3.0 7.5±3.1 -1.137 0.257 住院时间/d 10.0±3.2 11.0±3.4 -1.901 0.059 药物使用情况 ACEI/ARB 54(68.4) 68(67.3) 0.021 0.884 利尿剂 43(54.4) 62(61.4) 0.882 0.348 β受体阻滞剂 47(59.5) 54(53.4) 0.654 0.419 螺内酯 28(35.4) 29(28.7) 0.928 0.335 二甲双胍 47(59.5) 55(54.5) 0.458 0.498 胰岛素 31(39.2) 35(34.7) 0.402 0.526 胰岛素促泌剂 23(29.1) 21(20.8) 1.662 0.197 α-糖苷酶抑制剂 34(43.0) 34(33.7) 1.657 0.198 噻唑烷二酮类 15(19.0) 14(13.9) 0.862 0.353 二肽基肽酶Ⅳ抑制剂 17(21.5) 13(12.9) 2.387 0.122 表 2 随访12个月检验结果及临床事件
Table 2. 12-months followed up of inspection results and clinical events
例(%), X±S 项目 恩格列净组
(79例)对照组
(101例)t/χ2 P 糖化血红蛋白/% 6.7±0.5 6.8±0.5 -2.147 0.033 LVEF/% 55.3±5.9 53.4±6.3 2.061 0.041 心衰再入院 8(10.1) 21(20.8) 3.731 0.053 全因死亡 7(8.9) 16(15.8) 1.938 0.164 表 3 心衰再入院的多因素Cox回归分析
Table 3. multivariate Cox regression analysis of rehospitalization for heart failure
变量 B SE Wald P OR 95%CI 恩格列净 -0.922 0.467 3.902 0.048 0.398 0.159~0.993 慢性肾功能不全 1.151 0.493 5.446 0.020 3.163 1.202~8.318 缺血性心脏病 1.213 0.519 5.462 0.019 3.364 1.216~9.302 -
[1] 中国医疗保健国际交流促进会急诊医学分会, 中华医学会急诊医学分会, 中国医师协会急诊医师分会, 等. 中国脓毒症早期预防与阻断急诊专家共识[J]. 临床急诊杂志, 2020, 21(7): 517-529. https://www.cnki.com.cn/Article/CJFDTOTAL-ZZLC202007001.htm
[2] Jones TW, Smith SE, Van Tuyl JS, et al. Sepsis With Preexisting Heart Failure: Management of Confounding Clinical Features[J]. J Intensive Care Med, 2021, 36(9): 989-1012. doi: 10.1177/0885066620928299
[3] Abou Dagher G, Hajjar K, Khoury C, et al. Outcomes of patients with systolic heart failure presenting with sepsis to the emergency department of a tertiary hospital: a retrospective chart review study from Lebanon[J]. BMJ Open, 2018, 8(7): e022185. doi: 10.1136/bmjopen-2018-022185
[4] 刘德平. 钠-葡萄糖共转运蛋白2抑制剂在心力衰竭中的作用[J]. 中国心血管杂志, 2020, 25(1): 1-3. https://www.cnki.com.cn/Article/CJFDTOTAL-XIXG202001003.htm
[5] 中国医师协会急诊医师分会, 中国研究型医院学会休克与脓毒症专业委员会. 中国脓毒症/脓毒性休克急诊治疗指南(2018)[J]. 临床急诊杂志, 2018, 19(9): 567-588. https://www.cnki.com.cn/Article/CJFDTOTAL-ZZLC201809001.htm
[6] 马亮, 关晓楠, 刘文婷, 等. 伊伐布雷定在脓毒症合并急性心力衰竭易损期患者中应用1年随访疗效分析[J]. 中国急救医学, 2021, 41(9): 759-763. doi: 10.3969/j.issn.1002-1949.2021.09.005
[7] 中华医学会糖尿病学分会. 中国2型糖尿病防治指南(2020年版)[J]. 中华糖尿病杂志, 2021, 13(4): 315-409. https://www.cnki.com.cn/Article/CJFDTOTAL-ZZXJ202106003.htm
[8] Frydrych LM, Bian G, O'Lone DE, et al. Obesity and type 2 diabetes mellitus drive immune dysfunction, infection development, and sepsis mortality[J]. J Leukoc Biol, 2018, 104(3): 525-534. doi: 10.1002/JLB.5VMR0118-021RR
[9] Akinosoglou K, Kapsokosta G, Mouktaroudi M, et al. Diabetes on sepsis outcomes in non-ICU patients: A cohort study and review of the literature[J]. J Diabetes Complications, 2021, 35(1): 107765. doi: 10.1016/j.jdiacomp.2020.107765
[10] Arfaras-Melainis A, Polyzogopoulou E, Triposkiadis F, et al. Heart failure and sepsis: practical recommendations for the optimal management[J]. Heart Fail Rev, 2020, 25(2): 183-194. doi: 10.1007/s10741-019-09816-y
[11] Lee M, Brooksbank K, Wetherall K, et al. Effect of Empagliflozin on Left Ventricular Volumes in Patients With Type 2 Diabetes, or Prediabetes, and Heart Failure With Reduced Ejection Fraction(SUGAR-DM-HF)[J]. Circulation, 2021, 143(6): 516-525. doi: 10.1161/CIRCULATIONAHA.120.052186
[12] Packer M, Anker SD, Butler J, et al. Cardiovascular and Renal Outcomes with Empagliflozin in Heart Failure[J]. N Engl J Med, 2020, 383(15): 1413-1424. doi: 10.1056/NEJMoa2022190
[13] Shimizu W, Kubota Y, Hoshika Y, et al. Effects of empagliflozin versus placebo on cardiac sympathetic activity in acute myocardial infarction patients with type 2 diabetes mellitus: the EMBODY trial[J]. Cardiovasc Diabetol, 2020, 19(1): 148. doi: 10.1186/s12933-020-01127-z
[14] 廖梦阳, 廖玉华, 余淼, 等. SGLT2抑制剂治疗心力衰竭潜在机制的新认识[J]. 临床心血管病杂志, 2022, 38(1): 1-6. https://www.cnki.com.cn/Article/CJFDTOTAL-LCXB202201001.htm
[15] Hernandez M, Sullivan RD, McCune ME, et al. Sodium-Glucose Cotransporter-2 Inhibitors Improve Heart Failure with Reduced Ejection Fraction Outcomes by Reducing Edema and Congestion[J]. Diagnostics(Basel), 2022, 12(4).
[16] Zhao Y, Xu L, Tian D, et al. Effects of sodium-glucose co-transporter 2(SGLT2) inhibitors on serum uric acid level: A meta-analysis of randomized controlled trials[J]. Diabetes Obes Metab, 2018, 20(2): 458-462. doi: 10.1111/dom.13101
[17] Anker SD, Butler J, Filippatos G, et al. Empagliflozin in Heart Failure with a Preserved Ejection Fraction[J]. N Engl J Med, 2021, 385(16): 1451-1461. doi: 10.1056/NEJMoa2107038
[18] Packer M, Butler J, Zannad F, et al. Effect of Empagliflozin on Worsening Heart Failure Events in Patients With Heart Failure and Preserved Ejection Fraction: EMPEROR-Preserved Trial[J]. Circulation, 2021, 144(16): 1284-1294. doi: 10.1161/CIRCULATIONAHA.121.056824
-




 下载:
下载: