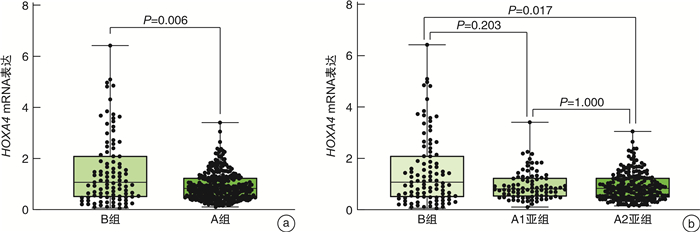
Correlation between HOXA4 gene expression in peripheral blood in patients with coronary heart disease and cardiovascular risk factors and characteristics of coronary artery lesions
-
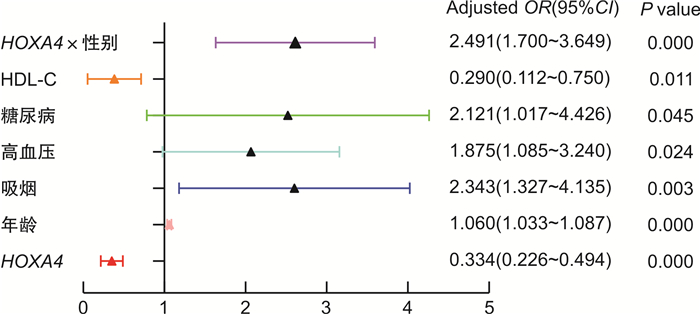
摘要: 目的 分析冠心病(CHD)患者外周血中同源框A4基因( HOXA4 )表达及心血管病危险因素与CHD病变特点的相关性。方法 纳入2021年11月1日—2022年1月31日连续在我院心脏介入中心行冠状动脉造影(CAG)的患者395例,其中确诊CHD 295例(A组),排除CHD 100例(B组)。据CAG结果将A组分为2个亚组,即中度狭窄组(A1亚组)和重度狭窄组(A2亚组)。CAG前收集外周动脉血3 mL检测 HOXA4 mRNA表达并记录患者血糖、血压及血脂等心血管病危险因素。比较组间 HOXA4 表达差异,逻辑回归分析 HOXA4 、心血管病危险因素与CHD病变特点的相关性。结果 HOXA4 在A组和A2亚组的表达低于B组(P<0.05)。 HOXA4 及高密度脂蛋白胆固醇(HDL-C)与CHD呈负相关(Adjusted OR < 1,P<0.05),年龄、吸烟、高血压及糖尿病与CHD呈正相关(Adjusted OR>1,P<0.05)。以B组为对照, HOXA4 表达、HDL-C水平与冠脉中、重狭窄呈负相关(Adjusted OR < 1,P<0.05);增龄与冠脉中、重度狭窄呈正相关(Adjusted OR>1,P<0.05);吸烟、糖尿病与冠脉重度狭窄呈正相关(Adjusted OR>1,P<0.05);高血压与冠脉中度狭窄呈正相关(Adjusted OR>1,P<0.05)。结论 HOXA4 低表达、低水平HDL-C、增龄、吸烟、高血压及糖尿病是CHD的危险因素,其中 HOXA4 低表达、低水平HDL-C及增龄与冠脉中、重度狭窄相关,吸烟、糖尿病与冠脉重度狭窄相关,而高血压与冠脉中度狭窄相关。Abstract: Objective To analyze the expression of homeobox A4 gene(HOXA4) in peripheral blood of patients with coronary heart disease(CHD) and the correlation between cardiovascular risk factors and characteristics of coronary artery lesions.Methods The 395 patients who underwent continuous coronary angiography in the Cardiac Intervention Center in our Hospital from November 01, 2021 to January 31, 2022 were selected. Among them, 295 patients were diagnosed definitely with CHD by CAG(Group A), and 100 patients without CHD(Group B). According to the results of CAG, Group A were divided into two subgroups: moderate stenosis group(Subgroup A1) and severe stenosis group(Subgroup A2). The 3 mL arterial blood was extracted from peripheral arteries before CAG to detect the mRNA expression of HOXA4 and recording clinical risk factors such as blood glucose, blood pressure, and lipids of the patient. The difference of HOXA4 expression between each groups was compared by non-parametric test, and the correlation between HOXA4, cardiovascular risk factors and characteristics of coronary artery lesions was analyzed by logistic regression.Results The expression of HOXA4 in Group A and Subgroup A2 were lower than that in Group B(P < 0.05). HOXA4 and HDL-C were negatively correlated with CHD(Adjusted OR < 1, P < 0.05), age, smoking, hypertension and diabetes were positively correlated with CHD(Adjusted OR>1, P < 0.05). Compared with Group B, the expression of HOXA4 and HDL-C level were negatively correlated with moderate and severe coronary artery stenosis(Adjusted OR < 1, P < 0.05). There was a positive correlation between aging and moderate and severe coronary artery stenosis(Adjusted OR>1, P < 0.05). Smoking and diabetes were positively correlated with severe coronary artery stenosis(Adjusted OR>1, P < 0.05). Hypertension was positively correlated with moderate coronary artery stenosis(Adjusted OR>1, P < 0.05).Conclusion Low expression of HOXA4, low level of HDL-C, aging, smoking, hypertension and diabetes were the risk factors of CHD, among which low expression of HOXA4, low level of HDL-C and aging were related to moderate and severe coronary artery stenosis, smoking and diabetes were related to severe coronary artery stenosis, while hypertension was related to moderate coronary artery stenosis.
-

-
表 1 A组和B组间心血管病危险因素比较
Table 1. Comparison of cardiovascular risk factors between Group A and Group B
例(%), M(P25, P75) 变量 A组(295例) B组(100例) P 男性 223(75.60) 49(49.00) <0.001 年龄/岁 65.00(56.00,72.00) 57.00(50.00,66.75) <0.001 吸烟 145(49.15) 37(37.00) 0.035 高血压 189(64.07) 44(44.00) <0.001 糖尿病 79(26.78) 12(12.00) 0.002 TG/(mmol/L) 1.53(1.09,2.54) 1.43(1.01,2.27) 0.405 LDL-C/(mmol/L) 2.42(1.80,3.08) 2.40(1.88,2.97) 0.724 HDL-C/(mmol/L) 0.93(0.80,1.07) 1.01(0.86,1.20) 0.002 TC/(mmol/L) 3.86(3.03,4.54) 3.83(3.13,4.46) 0.748 Scr/(mmol/L) 78.8(65.00,91.00) 72(57.00,85.75) 0.008 表 2 CHD危险因素的logistic回归分析
Table 2. Logistic regression analysis of cardiovascular risk factors in coronary heart disease
变量 P Crude OR(95%CI) Adjusted OR(95%CI) P HOXA4 0.001 0.634(0.491~0.820) 0.651(0.511~0.830) 0.001 男性 <0.001 3.244(2.008~5.176) 3.390(1.964~5.850) <0.001 年龄 <0.001 1.066(1.036~1.098) 1.060(1.034~1.087) <0.001 吸烟 0.006 2.454(1.297~4.642) 2.206(1.262~3.857) 0.006 高血压 0.010 2.208(1.206~4.043) 1.756(1.024~3.011) 0.041 糖尿病 0.041 2.233(1.034~4.821) 2.183(1.044~4.568) 0.038 HDL-C 0.003 0.165(0.051~0.536) 0.283(0.109~0.734) 0.005 表 3 CHD危险因素的分层研究及交互作用检测
Table 3. Stratified study and interaction detection of risk factors of coronary heart disease
变量 OR(95%CI) P 交互P 性别 0.014 男性 0.792(0.600~1.044) 0.098 女性 0.400(0.293~0.671) 0.001 吸烟 0.079 无 0.724(0.569~0.921) 0.009 有 0.438(0.254~-0.756) 0.003 高血压 0.889 无 0.695(0.468~1.033) 0.072 有 0.661(0.488~0.895) 0.007 糖尿病 0.091 无 0.539(0.391~0.744) <0.001 有 0.852(0.570~1.273) 0.435 年龄 0.557 青中年 0.647(0.414~1.013) 0.057 老年 0.639(0.460~0.886) 0.007 HDL-C 0.043 正常 0.657(0.505~0.853) 0.002 异常 0.334(0.082~1.362) 0.126 表 4 HOXA 4及心血管病危险因素与冠脉狭窄程度
Table 4. Correlation between HOXA 4, cardiovascular risk factors and degree of coronary artery stenosis
组别 变量 P Crude OR(95%CI) Adjusted OR(95%CI) P A1亚组 HOXA4 0.036 0.731(0.546~0.980) 0.751(0.585~0.963) 0.024 HDL-C 0.010 0.228(0.074~0.700) 0.152(0.042~0.559) 0.005 年龄 <0.001 1.068(1.038~1.098) 1.076(1.042~1.111) <0.001 男性 <0.001 4.749(2.434~9.263) 5.292(2.536~11.044) <0.001 吸烟 0.520 1.212(0.675~2.175) 1.464(0.755~2.836) 0.259 高血压 <0.001 3.876(2.079~7.225) 3.045(1.547~5.992) 0.001 糖尿病 0.004 3.026(1.420~6.450) 2.127(0.936~4.833) 0.072 A2亚组 HOXA4 <0.001 0.537(0.400~0.722) 0.570(0.424~0.767) <0.001 HDL-C 0.007 0.318(0.138~0.736) 0.301(0.114~0.797) 0.016 年龄 <0.001 1.040(1.017~1.064) 1.054(1.027-1.082) <0.001 男性 <0.001 2.788(1.694~4.587) 3.412(1.979~5.884) <0.001 吸烟 0.012 1.876(1.150~3.061) 2.064(1.187~3.590) 0.010 高血压 0.013 1.848(1.141~2.996) 1.611(0.934~2.780) 0.087 糖尿病 0.007 2.540(1.288~5.010) 2.176(1.041~4.550) 0.039 -
[1] 李建军, 杨进刚. "融合"学说: 胆固醇、炎症与动脉粥样硬化的新视野[J]. 临床心血管病杂志, 2022, 38(4): 265-266. https://lcxxg.whuhzzs.com/article/doi/10.13201/j.issn.1001-1439.2022.04.002
[2] 田嘉珉, 陈羽斐, 沈伟. M2型巨噬细胞极化及其对动脉粥样硬化的影响[J]. 临床心血管病杂志, 2022, 38(10): 838-843. https://lcxxg.whuhzzs.com/article/doi/10.13201/j.issn.1001-1439.2022.10.016
[3] Lillvis JH, Erdman R, Schworer CM, et al. Regional expression of HOXA4 along the aorta and its potential role in human abdominal aortic aneurysms[J]. BMC Physiol, 2011, 11: 9. doi: 10.1186/1472-6793-11-9
[4] Kimura M, Horie T, Baba O, et al. Homeobox A4 suppresses vascular remodeling by repressing YAP/TEAD transcriptional activity[J]. EMBO Rep, 2020, 21(4): e48389. doi: 10.15252/embr.201948389
[5] Liu NM, Yokota T, Maekawa S, et al. Transcription profiles of endothelial cells in the rat ductus arteriosus during a perinatal period[J]. PLoS One, 2013, 8(9): e73685. doi: 10.1371/journal.pone.0073685
[6] Aonuma T, Moukette B, Kawaguchi S, et al. MiR-150 attenuates maladaptive cardiac remodeling mediated by long noncoding RNA MIAT and directly represses profibrotic Hoxa4[J]. Circ Heart Fail, 2022, 15(4): e008686.
[7] Milcent C, Dormont B, Durand-Zaleski I, et al. Gender differences in hospital mortality anduse of percutaneous coronary intervention in acute myocardial infarction: microsimulation analysis of the 1999 nationwide French hospitals database[J]. Circulation, 2007, 115(7): 833-839. doi: 10.1161/CIRCULATIONAHA.106.664979
[8] Hao Y, Liu J, Liu J, et al. Sex differences in in-hospital management and outcomes of patients with acute coronary syndrome[J]. Circulation, 2019, 139(15): 1776-1785. doi: 10.1161/CIRCULATIONAHA.118.037655
[9] Matova EE, Vihert AM. Atherosclerosis and hypertension[J]. Bull World Health Organ, 1976, 53(5-6): 539-546.
[10] Chen S, Shen Y, Liu YH, et al. Impact of glycemic control on the association of endothelial dysfunction and coronary artery disease in patients with type 2 diabetes mellitus[J]. Cardiovasc Diabetol, 2021, 20(1): 64.
-




 下载:
下载: