Concomitant surgical interventions for preoperative mitral regurgitation with left ventricular assist device implantation: a meta-analysis
-
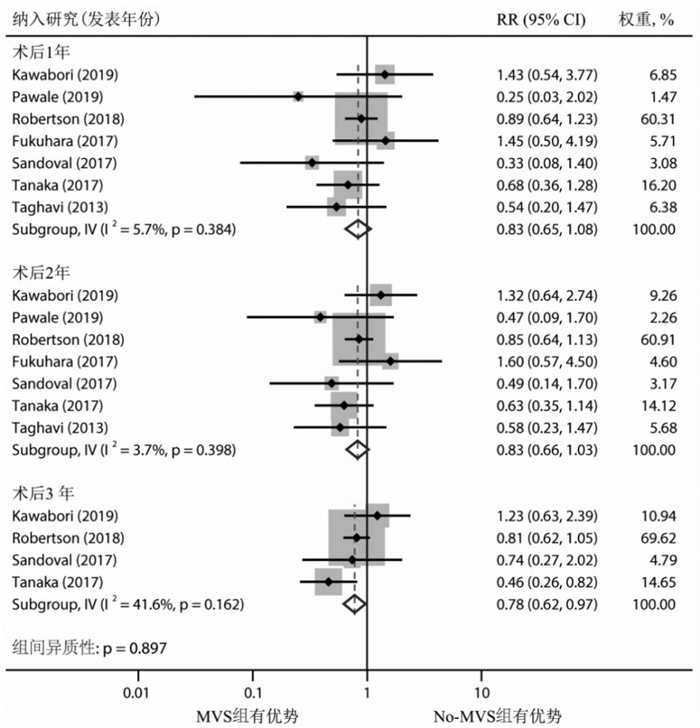
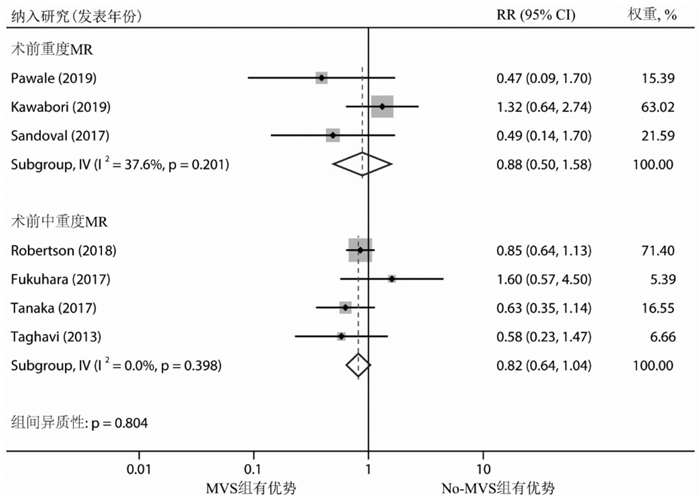
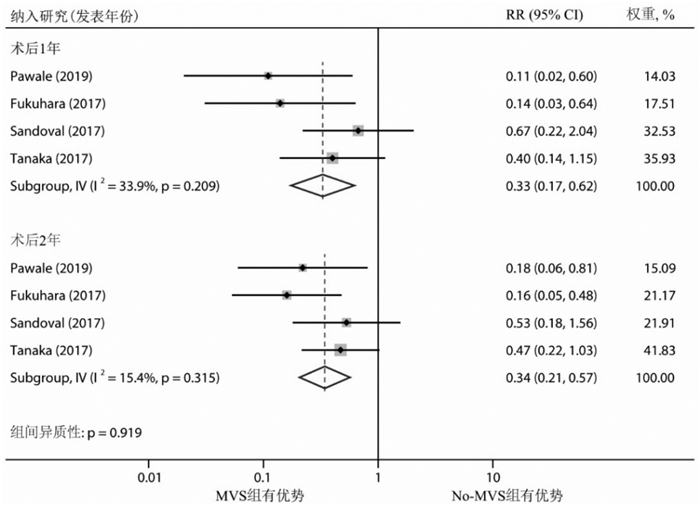
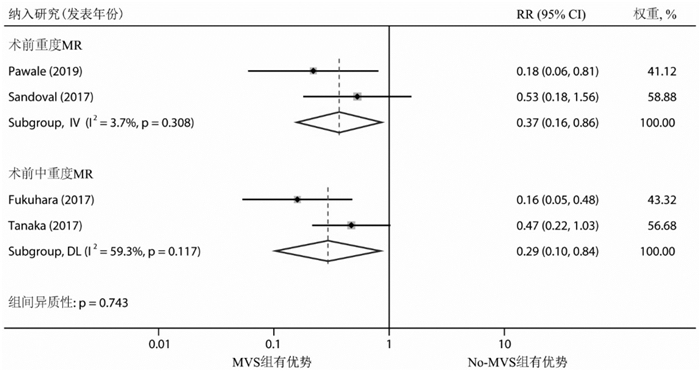
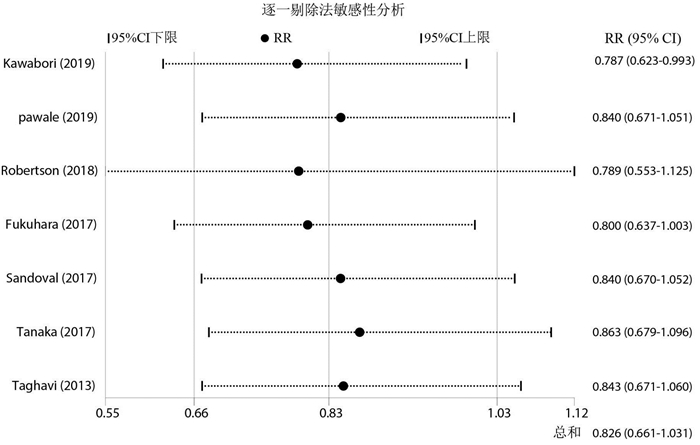
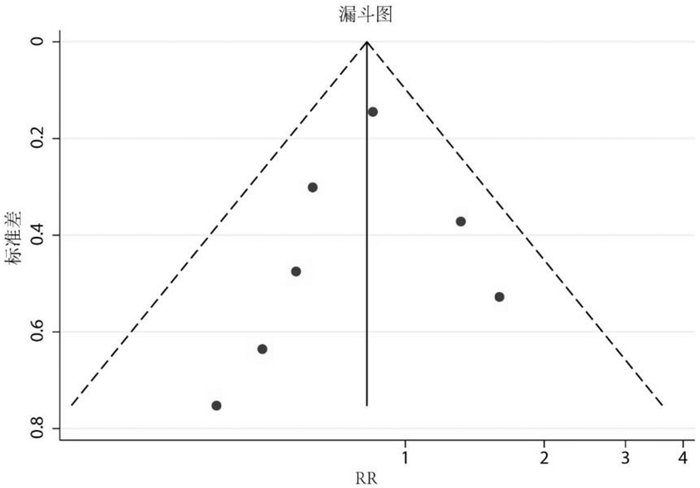
摘要: 目的 评价左心室辅助装置(left ventricular assist device,LVAD)植入同期行二尖瓣手术(mitral valve surgery,MVS)干预术前严重二尖瓣反流(mitral regurgitation,MR)对临床预后的影响。方法 检索PubMed、Embase、Cochrane Library、Web of Science数据库中建库起至2022年10月10日关于比较LVAD植入是否同期行MVS干预术前MR的文献。主要研究终点为全因死亡率,次要终点为术后MR复发、再入院等并发症。采用STATA 15.1软件进行统计学分析。结果 最终纳入7项回顾性队列研究,共5 504例患者,仅517例(9.4%)同期行MVS。荟萃分析显示,同期行MVS没有增加术后近、中期死亡率,MVS组、No-MVS组术后30 d全因死亡率分别为4.3%、4.9%;MVS组术后1年(RR=0.83,95%CI:0.65~1.08,P=0.384)、2年(RR=0.83,95%CI:0.66~1.03,P=0.446)和3年(RR=0.78,95%CI:0.62~0.97,P=0.162)全因死亡风险有下降趋势,但差异无统计学意义。同期行MVS没有增加术后中远期再入院的风险,MVS组术后1年(RR=0.33,95%CI:0.17~0.62,P=0.209)、2年(RR=0.34,95%CI:0.21~0.57,P=0.315)因心力衰竭再入院的风险明显下降,但差异无统计学意义。结论 LVAD植入同期行MVS干预术前严重的MR是安全可行的,没有增加术后近中期全因死亡率和再入院率,似乎可以降低术后中远期全因死亡和再入院的风险。Abstract: Objective To evaluate the impact of left ventricular assist device(LVAD) implantation concomitant with mitral valve surgery(MVS) to intervene in preoperative significant mitral regurgitation(MR) on clinical prognosis.Methods The PubMed, Embase, Cochrane Library, and Web of Science databases were searched for literature on comparing LVAD implantation with or without concomitant MVS intervention for preoperative MR from inception to 10 October 2022. The primary study endpoint was all-cause mortality, and secondary endpoints were complications such as postoperative MR recurrence and readmission. Statistical analysis was performed using STATA 15.1 software.Results A total of 7 retrospective cohort studies with 5 500 patients were included, and only 517(9.4%) patients received concomitant MVS. Meta-analysis showed that concomitant MVS did not increase postoperative early and mid-term mortality, with all-cause mortality rates of 4.3% and 4.9% at 30 days postoperatively in the MVS and No-MVS groups, respectively. There was a trend towards a decreased risk of all-cause mortality in the MVS group at 1 year(RR=0.83, 95%CI: 0.65-1.08, P=0.384), 2 years(RR=0.83, 95%CI: 0.66-1.03, P=0.446), and 3 years(RR=0.78, 95%CI: 0.62-0.97, P=0.162) after surgery, but the differences were not statistically significant. Concomitant MVS did not increase the risk of mid-to long-term postoperative readmission, and the risk of readmission for heart failure was lower in the MVS group at 1 year(RR=0.33, 95%CI: 0.17-0.62, P=0.209) and 2 years(RR=0.34, 95%CI: 0.21-0.57, P=0.315) after surgery, but the differences were not statistically significant.Conclusion Concomitant MVS with LVAD implantation to intervene preoperative severe MR is safe and feasible, which does not increase the rate of early and mid-term postoperative all-cause mortality and readmission, and seems to reduce the risk of mid to long-term all-cause mortality and readmission.
-

-
表 1 纳入研究的基本特征
Table 1. Basic characteristics of included studies
研究 国家 研究时间 术前MR程度 样本量(MVS组/No-MVS组)/例 LVAD类型 NOS评分 Pawale 2019[14] 美国 2011—2017年 重度 78/28 HMⅡ 89.3%,HVAD 6.0%,
HMⅢ 4.7%8 Kawabori 2019[15] 美国 2003—2016年 重度 26/82 HMⅡ 79例(73.1%),HVAD 29例(26.9%) 7 Robertson 2018[6] 美国 2008—2014年 中重度 263/4 667 NR 7 Sandoval 2017[17] 美国 1999—2013年 重度 21/57 NR 8 Fukuhara 2017[18] 美国 2004—2014年 中重度 52/63 HMⅡ 86例(74.8%),HVAD 21例(18.3%),其他8例(6.9%) 8 Tanaka 2017[16] 美国 2008—2014年 中重度 56/54 HMⅡ110例(100%) 8 Taghavi 2013[19] 美国 2009—2011年 中重度 21/36 HMⅡ57例(100%) 7 HMⅡ:HeartMate Ⅱ;HMⅢ:HeartMate Ⅲ;NR:未报道。 表 2 两组术后30 d死亡率比较
Table 2. Comparison of 30-day postoperative mortality
研究 组别 样本量/例 死亡/例(%) Pawale 2019 MVS组 78 2(2.6) No-MVS组 28 1(3.6) Robertson 2018 MVS组 263 13(5.0) No-MVS组 4 667 233(5.0) Fukuhara 2017 MVS组 52 2(3.8) No-MVS组 63 0 总计 MVS组 393 17(4.3) No-MVS组 4 758 234(4.9) -
[1] 王华, 刘宇佳, 杨杰孚. 心力衰竭流行病学[J]. 临床心血管病杂志, 2023, 39(4): 243-247. https://lcxxg.whuhzzs.com/article/doi/10.13201/j.issn.1001-1439.2023.04.001
[2] 董念国. 浅谈心室辅助装置在终末期心力衰竭中的应用[J]. 临床心血管病杂志, 2023, 39(6): 409-412. https://lcxxg.whuhzzs.com/article/doi/10.13201/j.issn.1001-1439.2023.06.001
[3] Bragazzi NL, Zhong W, Shu J, et al. Burden of heart failure and underlying causes in 195 countries and territories from 1990 to 2017[J]. Eur J Prev Cardiol, 2021, 28(15): 1682-1690. doi: 10.1093/eurjpc/zwaa147
[4] Hao G, Wang X, Chen Z, et al. Prevalence of heart failure and left ventricular dysfunction in China: the China Hypertension Survey, 2012-2015[J]. Eur J Heart Fail, 2019, 21(11): 1329-1337. doi: 10.1002/ejhf.1629
[5] Jain R, Truby LK, Topkara VK. Residual mitral regurgitation in patients with left ventricular assist device support-An INTERMACS analysis[J]. J Heart Lung Transplant, 2022, 41(11): 1638-1645. doi: 10.1016/j.healun.2022.03.002
[6] Robertson JO, Naftel DC, Myers SL, et al. Concomitant mitral valve procedures in patients undergoing implantation of continuous-flow left ventricular assist devices: An INTERMACS database analysis[J]. J Heart Lung Transplant, 2018, 37(1): 79-88. doi: 10.1016/j.healun.2017.09.016
[7] Potapov EV, Antonides C, Crespo-Leiro MG, et al. 2019 EACTS Expert Consensus on long-term mechanical circulatory support[J]. Eur J Cardiothorac Surg, 2019, 56(2): 230-270. doi: 10.1093/ejcts/ezz098
[8] Feldman D, Pamboukian SV, Teuteberg JJ, et al. The 2013 International Society for Heart and Lung Transplantation Guidelines for mechanical circulatory support: Executive summary[J]. J Heart Lung Transplant, 2013, 32(2): 157-187. doi: 10.1016/j.healun.2012.09.013
[9] 郭颖, 张瑞生. 中国成人心脏瓣膜病超声心动图规范化检查专家共识[J]. 中国循环杂志, 2021, 36(2): 109-125.
[10] 赵恩慧, 黄丽红. 根据Kaplan-Meier曲线提取生存数据的系统化方法[J]. 中国循证医学杂志, 2022, 22(11): 1358-1364.
[11] Liu N, Zhou Y, Lee JJ. IPDfromKM: reconstruct individual patient data from published Kaplan-Meier survival curves[J]. BMC Med Res Methodol, 2021, 21(1): 111. doi: 10.1186/s12874-021-01308-8
[12] Guyot P, Ades AE, Ouwens MJ, et al. Enhanced secondary analysis of survival data: reconstructing the data from published Kaplan-Meier survival curves[J]. BMC Med Res Methodol, 2012, 12: 9. doi: 10.1186/1471-2288-12-9
[13] Stang A. Critical evaluation of the Newcastle-Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses[J]. Eur J Epidemiol, 2010, 25(9): 603-605. doi: 10.1007/s10654-010-9491-z
[14] Pawale A, Itagaki S, Parikh A, et al. Mitral valve repair for severe mitral valve regurgitation during left ventricular assist device implantation[J]. J Thorac Cardiovasc Surg, 2019, 157(5): 1841-1848. doi: 10.1016/j.jtcvs.2018.12.071
[15] Kawabori M, Kurihara C, Conyer RT, et al. Effect of concomitant mitral valve procedures for severe mitral regurgitation during left ventricular assist device implantation[J]. J Artif Organs, 2019, 22(2): 91-97. doi: 10.1007/s10047-018-1076-8
[16] Tanaka A, Onsager D, Song T, et al. Surgically Corrected Mitral Regurgitation During Left Ventricular Assist Device Implantation Is Associated With Low Recurrence Rate and Improved Midterm Survival[J]. Ann Thorac Surg, 2017, 103(3): 725-733. doi: 10.1016/j.athoracsur.2016.06.078
[17] Sandoval E, Singh SK, Carillo J A, et al. Impact of concomitant mitral valve repair for severe mitral regurgitation at the time of continuous-flow left ventricular assist device insertion[J]. Interact Cardiovasc Thorac Surg, 2017, 25(4): 620-623. doi: 10.1093/icvts/ivx223
[18] Fukuhara S, Takeda K, Chiuzan C, et al. Concomitant mitral repair and continuous-flow left ventricular assist devices: Is it warranted?[J]. J Thorac Cardiovasc Surg, 2017, 154(4): 1303-1312. doi: 10.1016/j.jtcvs.2017.04.021
[19] Taghavi S, Hamad E, Wilson L, et al. Mitral valve repair at the time of continuous-flow left ventricular assist device implantation confers meaningful decrement in pulmonary vascular resistance[J]. ASAIO J, 2013, 59(5): 469-473. doi: 10.1097/MAT.0b013e31829be026
[20] Saeed D, Feldman D, Banayosy A E, et al. The 2023 International Society for Heart and Lung Transplantation Guidelines for Mechanical Circulatory Support: A 10-Year Update[J]. J Heart Lung Transplant, 2023, 42(7): e1-e222. doi: 10.1016/j.healun.2022.12.004
[21] Stulak JM, Lee D, Haft JW, et al. Gastrointestinal bleeding and subsequent risk of thromboembolic events during support with a left ventricular assist device[J]. J Heart Lung Transplant, 2014, 33(1): 60-64. doi: 10.1016/j.healun.2013.07.020
[22] Schreiber C, Dieterlen MT, Garbade J, et al. Validation of mitral regurgitation reversibility in patients with HeartMate 3 LVAD implantation[J]. Artif Organs, 2022, 46(1): 106-116. doi: 10.1111/aor.14053
[23] 袁莉, 孙晓宁, 王春生. 左心室辅助装置置入术后右心衰的防治[J]. 中华胸心血管外科杂志, 2021, 37(12): 765-768.
[24] Pausch J, Bhadra O, Mersmann J, et al. Prognostic impact of functional mitral regurgitation prior to left ventricular assist device implantation[J]. J Cardiothorac Surg, 2022, 17(1): 24. doi: 10.1186/s13019-021-01748-9
[25] Zhou W, Du Z, Tao Y, et al. Effect of preoperative pulmonary artery pressure on the prognosis of end-stage heart failure patients after heart transplantation[J]. J Cardiothorac Surg, 2023, 18(1): 154-154. doi: 10.1186/s13019-023-02253-x
[26] Lee HW, Jung JW, Kim AY, et al. Heart Transplantation in a Patient with Complex Congenital Heart Disease, Physiologic Single Lung, and Severe Pulmonary Hypertension[J]. Yonsei Med J, 2022, 63(12): 1144-1146. doi: 10.3349/ymj.2022.0384
[27] Okoh A, Yanagida R, Schultheis M, et al. Impact of Baseline Mitral Regurgitation on Postoperative Outcomes After Left Ventricular Assist Device Implantation as Destination Therapy[J]. Transplant Proc, 2019, 51(5): 1636-1636. doi: 10.1016/j.transproceed.2019.04.017
[28] Kanwar MK, Rajagopal K, Itoh A, et al. Impact of left ventricular assist device implantation on mitral regurgitation: An analysis from the MOMENTUM 3 trial[J]. J Heart Lung Transplant, 2020, 39(6): 529-537. doi: 10.1016/j.healun.2020.03.003
[29] Kassis H, Cherukuri K, Agarwal R, et al. Significance of Residual Mitral Regurgitation After Continuous Flow Left Ventricular Assist Device Implantation[J]. JACC Heart Fail, 2017, 5(2): 81-88. doi: 10.1016/j.jchf.2016.09.014
-





 下载:
下载: